Indications
| Indication | Clinical Context |
|---|---|
| Refractory variceal hemorrhage | Esophageal or gastric varices with failed endoscopic and medical management; high-risk acute bleeding (Child-Pugh B with active bleeding or Child-Pugh C) — early TIPS within 72 h |
| Refractory ascites | Two or more large-volume paracenteses within 4 weeks despite maximum diuretic therapy; not first-line treatment for uncomplicated ascites |
| Hepatic hydrothorax | Refractory pleural effusion in cirrhotic patient after failed thoracentesis and medical therapy |
| Budd-Chiari syndrome | Acute or subacute hepatic vein obstruction with clinical decompensation; bridge to transplant |
| Ectopic or portal hypertensive varices | Stomal, rectal, or mesenteric varices causing bleeding not amenable to endoscopic treatment |
Contraindications
| Type | Contraindication |
|---|---|
| Absolute | Right heart failure (EF <20% or significant right ventricular dysfunction); severe pulmonary hypertension (PASP >45 mmHg); uncontrolled grade 3–4 hepatic encephalopathy; polycystic liver disease; active systemic infection or sepsis; severe uncorrected coagulopathy (INR >5) |
| Relative | Child-Pugh C (≥12) without bridging-to-transplant intent; bilirubin >3–5 mg/dL; MELD >24; hepatic neoplasm in planned shunt tract; biliary obstruction; prior hepatic encephalopathy (grade 3–4) |
Cardiac evaluation is mandatory: Echocardiography to assess right ventricular function and pulmonary artery pressure before every elective TIPS. The abrupt increase in central venous return from shunt creation can precipitate acute right heart failure in patients with borderline function. For borderline dysfunction (EF 20–35%), cardiology co-management is required.
Relevant Anatomy
Hepatic Vein to Portal Vein Relationships
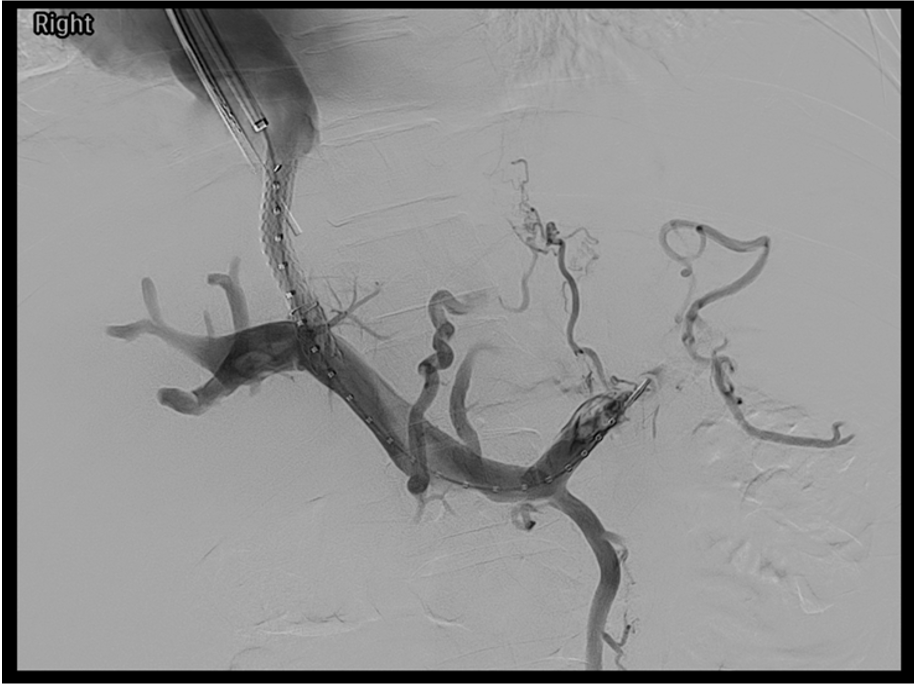
The TIPS shunt connects the hepatic venous system to the portal venous system through a tract created within the hepatic parenchyma. The right hepatic vein to right portal vein is the standard approach — it provides the most direct path and requires the shortest stent. The right main portal vein, just posterior to the hepatic artery bifurcation, is the standard portal vein target; its bifurcation serves as the primary fluoroscopic landmark.
The distance between the right hepatic vein and right portal vein is typically 3–5 cm in most patients. The middle hepatic vein to left portal vein tract is an alternative when right-sided anatomy is unfavorable, and is preferred for left-sided (gastric fundal) variceal bleeding.
Right IJV Access
The right internal jugular vein (IJV) is the preferred access site — the straighter path to the right atrium and inferior vena cava facilitates reliable hepatic vein selection and needle positioning. Left IJV access is technically more difficult due to the more tortuous course and should be avoided unless there is a specific indication.
Pre-Procedure Checklist
Imaging Review
- CT or MRI with contrast within 3 months: hepatic vein anatomy, portal vein patency, liver size and parenchymal quality, ascites volume, varices
- Confirm portal vein is patent — complete main portal vein thrombosis is a relative to absolute contraindication
- Identify any hepatic neoplasm in the planned shunt tract
Labs
- CBC, comprehensive metabolic panel, INR/PT, type and screen
- Target: platelets >50,000 (transfuse if needed); INR <2.5 (FFP or PCC if needed)
- Calculate MELD score and Child-Pugh class — document baseline
Cardiac Evaluation
- Echocardiogram to assess right ventricular function and pulmonary artery systolic pressure — mandatory before elective TIPS
- EF <20% or right heart failure: absolute contraindication
- Borderline dysfunction (EF 20–35%): formal cardiology consultation required; consider constrained-diameter shunt technique
Hepatic Encephalopathy Assessment
- Baseline neurologic exam; document any prior encephalopathy episodes
- Optimize lactulose and rifaximin pre-procedure in patients at elevated risk
- Prior grade 3–4 encephalopathy is the strongest predictor of post-TIPS encephalopathy
Consent Considerations
Discuss with the patient and family: new or worsening hepatic encephalopathy (20–30%), shunt dysfunction or thrombosis, hepatic decompensation, intra-abdominal bleeding (capsular perforation), biliary injury (hemobilia), contrast nephropathy, and the risk of procedure-related mortality (higher with acute high-risk bleeding, MELD ≥24, or Child-Pugh C).
Procedure Overview
The following is a high-level summary. Full step-by-step technique, equipment selection, and periprocedural management are available in RadCall Pro.
- Vascular access — ultrasound-guided right internal jugular vein access
- Hepatic vein selection — advance catheter and wire to select the target hepatic vein (right or middle); measure baseline hepatic vein and right atrial pressures
- Portal vein access — advance the TIPS needle set into the hepatic vein; puncture from hepatic vein into the portal vein under imaging guidance (fluoroscopy alone, or with intracardiac echocardiography for real-time visualization); confirm intraportal position by aspiration and small contrast injection showing portal branching
- Wire and sheath placement — advance wire into the portal system; upsize to working wire and sheath; perform portal venography and measure direct portal pressure
- Portosystemic gradient measurement — calculate PPG (portal pressure minus right atrial pressure); target <12 mmHg for variceal hemorrhage, <8 mmHg for refractory ascites
- Tract measurement and stent sizing — measure the parenchymal tract length to select correct stent size
- Covered stent deployment — advance the ePTFE-covered stent (Viatorr); the covered portion spans the liver parenchyma and uncovered portion extends 1–2 cm into the portal vein
- Post-dilation and final assessment — dilate deployed stent; repeat pressure measurements and portal venogram; embolize varices if indicated; document final PPG
Complications
| Complication | Rate | Recognition & Management |
|---|---|---|
| Hepatic encephalopathy | 20–30% new or worsening | Peak incidence in first months post-procedure; medical management first (lactulose, rifaximin); TIPS reducer device for refractory cases; shunt occlusion as last resort |
| Shunt stenosis or occlusion | <10% at 1 year (covered stent); 20–30% (bare metal) | Detected by Duplex ultrasound surveillance; recurrent symptoms (ascites return, variceal rebleed); managed by balloon angioplasty or parallel stent placement |
| Intra-abdominal hemorrhage | <1% | Capsular perforation or hepatic artery injury during parenchymal puncture; CT for characterization; selective embolization for arterial bleeding |
| Hepatic failure | Varies by baseline function | Acute decompensation from shunting of portal blood; higher risk with MELD ≥24 or Child-Pugh C; aggressive supportive care; liver transplant evaluation |
| Right heart failure exacerbation | Rare with proper screening | Sudden increase in preload; continuous hemodynamic monitoring; aggressive diuresis; vasopressors if unstable; prevented by pre-procedure cardiac evaluation |
| Biliary injury (hemobilia) | Rare | Intrahepatic bile duct puncture during needle pass; presents as hemobilia; may require ERCP or biliary drainage; stent infection risk |
Post-Procedure Care
Immediate Monitoring
- ICU or step-down unit for 24 hours after general anesthesia or complex cases
- Vital signs every 1 hour for 4 hours, then every 4 hours
- Neurologic checks every 4 hours for hepatic encephalopathy screening
- Labs at 6 hours post-procedure: CBC, comprehensive metabolic panel, liver function tests
Outpatient Surveillance
- Duplex ultrasound at 1 month, then every 6 months — standard TIPS surveillance to detect shunt stenosis before clinical failure
- MELD and Child-Pugh reassessment at 4–6 weeks post-procedure
- For TIPS placed for ascites: continue diuretics at reduced dose; allow 4–6 weeks for ascites to respond before judging efficacy
- Encephalopathy prophylaxis: lactulose titrated to 2–3 soft stools per day plus rifaximin in high-risk patients
When to Escalate
- New or worsening encephalopathy post-TIPS — optimize lactulose and rifaximin; if severe or refractory, interventional TIPS reduction with a reducer device; discuss with hepatology
- Recurrent variceal bleeding or reaccumulating ascites after TIPS — urgent Doppler ultrasound to assess shunt patency; shunt stenosis requires balloon angioplasty or restenting
- Signs of right heart failure post-procedure (hypotension, elevated JVP, worsening oxygen saturation) — IV diuresis; hemodynamic monitoring; urgent cardiology consultation
- Suspected intra-abdominal hemorrhage (pain, dropping hemoglobin) — urgent CT abdomen with contrast; interventional radiology or surgical consultation for active bleeding
Evidence Summary
The evidence for TIPS is robust across multiple indications. The strongest data support its use in preemptive TIPS for high-risk acute variceal bleeding (survival benefit in RCTs) and refractory ascites (improved transplant-free survival vs. LVP). Evidence for hepatorenal syndrome and hepatic hydrothorax is more limited.
1. Preemptive (Early) TIPS — Acute Variceal Bleeding
This indication has the strongest evidence, with multiple RCTs and meta-analyses demonstrating survival benefit in high-risk patients (Child-Pugh B with active bleeding or Child-Pugh C 10–13).
| Study | Design | Key Outcome |
|---|---|---|
| García-Pagán et al. (NEJM 2010) [1] | RCT, n=63, Child-Pugh B (active bleeding) or C (10–13) | Preemptive TIPS within 72 h: rebleeding 3% vs. 50%; 1-year mortality 14% vs. 39% (P<0.001) |
| IPD Meta-Analysis (Hepatology 2024) [2] | 2-stage IPD meta-analysis, 8 studies (4 RCTs + 4 observational), n=1,389 | 1-year mortality HR 0.43 (95% CI 0.32–0.60, P<0.001); benefit consistent across subgroups |
AASLD 2024 criteria for preemptive TIPS (within 24–72 h of initial endoscopy): Child-Pugh B score 8–9 with active bleeding at endoscopy; Child-Pugh C score 10–13; or HVPG >20 mmHg if measured. [3,4]
Exclusion criteria from RCTs: Age >75, HCC beyond early stage, severe renal disease, complete portal vein thrombosis, right heart failure, prior secondary prophylaxis, non-esophageal variceal source.
2. Secondary Prophylaxis of Variceal Bleeding
For survivors of an initial variceal bleed, TIPS is superior to endoscopic therapy + beta-blockers for preventing rebleeding, though a consistent survival benefit is not seen in all trials.
| Study | n | Key Outcome |
|---|---|---|
| Meta-analysis, 9 RCTs [5] | 608 | 1-year mortality RR 0.68 (95% CI 0.49–0.96); rebleeding RR 0.28 (0.20–0.40); hepatic encephalopathy not significantly increased (RR 1.36, 0.72–2.56) |
| Covered TIPS vs. EVL + beta-blocker [7] | 72 | Rebleeding 0% (TIPS) vs. 29% (EVL + BB; P=.001); no survival difference |
| 8-mm TIPS vs. EVL + propranolol (Radiology 2023) [8] | 100 (Child-Pugh B/C) | Rebleeding HR 0.31 (0.14–0.69); encephalopathy higher with TIPS (30% vs. 16%); no survival benefit |
3. Refractory and Recurrent Ascites
TIPS significantly improves ascites control and reduces portal hypertension-related events compared with large-volume paracentesis (LVP). Hepatic encephalopathy is the main trade-off.
| Study | Design | Key Outcome |
|---|---|---|
| Bureau et al. (Gastroenterology 2017) [9] | RCT, n=62, covered TIPS vs. LVP + albumin | 1-year transplant-free survival 93% vs. 52% (P=.003); 32 vs. 320 paracenteses; 0% vs. 18% portal hypertensive bleeding; encephalopathy similar (65% each group) |
| Meta-analysis, 5 RCTs [10] | 305 | Recurrent ascites 42% (TIPS) vs. 89% (LVP); 2-year mortality 51% vs. 65%; encephalopathy episodes 1.1 vs. 0.63/year |
| Multicenter observational (Int J Surg 2025) [11] | 462 | 1-year survival 77.9% (TIPS) vs. 47.3% (LVP + albumin; adjusted HR 0.43, 0.29–0.64); further paracentesis 17.9% vs. 100%; encephalopathy 26.5% vs. 6.4% |
The AGA 2025 Clinical Practice Update recommends referral for TIPS in well-selected patients with refractory ascites, hepatic hydrothorax, volume overload, or hyponatremia. [12]
4. Hepatorenal Syndrome (HRS)
Evidence is limited and of low certainty. A 2024 Cochrane Review of 2 RCTs (130 patients) comparing TIPS with conventional therapy (paracentesis + albumin) in HRS type 2 found uncertain effect on mortality (RR 0.88, 95% CI 0.55–1.38; very low-certainty evidence) and possible improvement in kidney function (RR 0.53, 0.27–1.02; low-certainty evidence). TIPS may be considered in HRS type 2 (chronic HRS-AKI) as it improves renal perfusion by reducing portal pressure, but current evidence does not support routine use. [13,14]
5. Hepatic Hydrothorax
Evidence is limited to observational data. TIPS reduces the transdiaphragmatic pressure gradient driving pleural fluid accumulation, with response rates similar to refractory ascites (~80% clearance). The AGA 2025 update recommends referral for TIPS in well-selected patients with refractory hepatic hydrothorax. [12,14]
6. Gastric Varices (GOV2/IGV1)
One RCT (72 patients) comparing TIPS with repeated cyanoacrylate injection for gastrofundal variceal rebleeding prevention showed lower rebleeding with TIPS but higher encephalopathy rates and no survival difference. TIPS is recommended among first-line options for secondary prophylaxis of gastrofundal variceal bleeding. [3]
Technical Evidence
| Topic | Evidence |
|---|---|
| Covered vs. bare metal stents | ePTFE-covered stents (Viatorr) have significantly lower shunt dysfunction rates (<10% at 1 year vs. 20–30% for bare metal); covered stents are standard of care [9] |
| Stent diameter (8 vs. 10 mm) | 8-mm stents reduce hepatic encephalopathy without compromising ascites control; used preferentially in encephalopathy-risk patients [15] |
| Rifaximin prophylaxis | RCT evidence supports prophylactic rifaximin to reduce post-TIPS hepatic encephalopathy [12,4] |
| Prognostic scoring (FIPS) | The Freiburg Index of Post-TIPS Survival (FIPS) and age-specific models predict post-TIPS mortality and guide patient selection [16] |
References
- García-Pagán JC, Caca K, Bureau C, et al. Early use of TIPS in patients with cirrhosis and variceal bleeding. N Engl J Med. 2010;362(25):2370–2379.
- Nicoară-Farcău O, Han G, Rudler M, et al. Pre-emptive TIPS in high-risk acute variceal bleeding: an updated and revised individual patient data meta-analysis. Hepatology. 2024;79(3):624–635.
- Lee EW, Eghtesad B, Garcia-Tsao G, et al. AASLD practice guidance on the use of TIPS, variceal embolization, and retrograde transvenous obliteration in the management of variceal hemorrhage. Hepatology. 2024;79(1):224–250.
- Kaplan DE, Ripoll C, Thiele M, et al. AASLD practice guidance on risk stratification and management of portal hypertension and varices in cirrhosis. Hepatology. 2024;79(5):1180–1211.
- Halabi SA, Sawas T, Sadat B, et al. Early TIPS versus endoscopic therapy for secondary prophylaxis after management of acute esophageal variceal bleeding in cirrhotic patients: a meta-analysis of randomized controlled trials. J Gastroenterol Hepatol. 2016;31(9):1519–1526.
- Nanchal R, Subramanian R, Alhazzani W, et al. Guidelines for the management of adult acute and acute-on-chronic liver failure in the ICU. Crit Care Med. 2023;51(5):657–676.
- Holster IL, Tjwa ET, Moelker A, et al. Covered transjugular intrahepatic portosystemic shunt versus endoscopic therapy + β-blocker for prevention of variceal rebleeding. Hepatology. 2016;63(2):581–589.
- Wang X, Liu G, Wu J, et al. Small-diameter transjugular intrahepatic portosystemic shunt versus endoscopic variceal ligation plus propranolol for variceal rebleeding in advanced cirrhosis. Radiology. 2023;308(2):e223201.
- Bureau C, Thabut D, Oberti F, et al. Transjugular intrahepatic portosystemic shunts with covered stents increase transplant-free survival of patients with cirrhosis and recurrent ascites. Gastroenterology. 2017;152(1):157–163.
- Tapper EB, Parikh ND. Diagnosis and management of cirrhosis and its complications: a review. JAMA. 2023;329(18):1589–1602.
- Wang B, Zhu J, Li J, et al. TIPS improves survival in patients with cirrhosis and recurrent ascites: a multicenter observational study. Int J Surg. 2025. doi:10.1097/JS9.0000000000004579.
- Orman ES, Fortune BE, John BV, Asrani SK. AGA clinical practice update on the management of ascites, volume overload, and hyponatremia in cirrhosis: expert review. Gastroenterology. 2025;169(7):1547–1557.
- Gonzalez-Garay AG, Serralde-Zúñiga AE, Velasco Hidalgo L, et al. Transjugular intrahepatic portosystemic shunts for adults with hepatorenal syndrome. Cochrane Database Syst Rev. 2024;1:CD011039.
- Rössle M, Gerbes AL. TIPS for the treatment of refractory ascites, hepatorenal syndrome and hepatic hydrothorax: a critical update. Gut. 2010;59(7):988–1000.
- Biggins SW, Angeli P, Garcia-Tsao G, et al. Diagnosis, evaluation, and management of ascites, spontaneous bacterial peritonitis and hepatorenal syndrome: 2021 practice guidance by AASLD. Hepatology. 2021;74(2):1014–1048.
- Bettinger D, Thimme R, Schultheiß M. Implantation of transjugular intrahepatic portosystemic shunt (TIPS): indication and patient selection. Curr Opin Gastroenterol. 2022;38(3):221–229.