Indications
| Indication | Details |
|---|---|
| Osteoporotic VCF | Primary indication — acute (<6 weeks) preferred; subacute (<3 months) acceptable when MRI STIR edema present |
| Malignant fracture | Myeloma, lytic metastases; consider ablation (coblation/RFA) before cement in highly vascular tumors (e.g., renal cell) |
| Painful vertebral hemangioma | Aggressive intraosseous hemangioma with refractory pain |
| Traumatic fracture | Non-osteoporotic acute fracture with significant pain refractory to conservative management |
Contraindications
| Type | Contraindication |
|---|---|
| Absolute | Stable, asymptomatic fracture · Active local or systemic infection · Neurologic deficit from retropulsed bony fragment (surgical or kyphoplasty preferred) · Uncorrectable coagulopathy · PMMA allergy |
| Relative | Vertebra plana (>75% height loss) — challenging but feasible; SpineJack preferred · Posterior wall disruption with canal compromise · Significant spinal instability requiring surgery |
Vertebroplasty vs. Kyphoplasty vs. SpineJack
| Feature | Vertebroplasty | Balloon Kyphoplasty | SpineJack |
|---|---|---|---|
| Mechanism | Direct cement injection | Balloon creates cavity → cement | Titanium implant expands craniocaudally → cement |
| Height restoration | Minimal | Moderate (balloon inflation) | Superior — up to 40% height gain; durable |
| Cement leak risk | Higher (no cavity) | Lower (contained cavity) | Low (implant contains cement) |
| Sedation | MAC / Local | MAC / General | General / MAC |
| Cost | Lowest | Moderate | Highest |
| Best for | VCF without significant height loss; malignant fractures | Height loss >15%; intact posterior wall; cavity containment desired | Acute fractures with significant height loss; young patients; durable restoration |
Relevant Anatomy
Transpedicular Approach (Standard)
The most common approach — viable when pedicle width ≥4–5 mm (standard for T4–L5). The needle trajectory runs along the posterior element through the pedicle into the vertebral body. Target: anteromedial one-third of the vertebral body (anterior 1/3 on lateral view, midline on AP). Bilateral bipedicular access is most common; unipedicular can achieve adequate midline fill for osteoporotic fractures.
Extrapedicular/Parapedicular Approach
Used when pedicles are too narrow — typically above T8 where pedicle width narrows to <4 mm. Needle passes lateral to the pedicle through the costovertebral junction (thoracic). Greater pneumothorax risk at upper thoracic levels.
Pedicle Width Reference
| Level | Pedicle Width | Approach |
|---|---|---|
| Upper thoracic (T1–T4) | 4–6 mm | Borderline; extrapedicular often safer |
| Mid-thoracic (T5–T10) | 5–8 mm | Transpedicular feasible; confirm on CT |
| Thoracolumbar (T11–L2) | 8–14 mm | Comfortable transpedicular access |
| Lumbar (L3–L5) | 12–20 mm | Widest; easiest transpedicular access |
Pre-Procedure Checklist
- MRI spine with STIR: STIR hyperintensity = bone marrow edema = active fracture that will respond. T1 hypointensity corroborates. If MRI contraindicated: bone scan (Tc-99m) to confirm activity. CT alone is insufficient.
- CT spine: Fracture morphology, posterior wall integrity, degree of height loss (Genant Grade 1 = 20–25%, Grade 2 = 25–40%, Grade 3 = >40%), pedicle width, canal compromise, fragment retropulsion
- Identify the symptomatic level: Correlate pain location with imaging — count from C2 or sacrum on sagittal MRI
- Labs: INR ≤1.5, platelets ≥50K (SIR Category 2). Hold anticoagulants per SIR guidelines.
- PMMA cement system confirmed available — Confidence, Vertas, or equivalent; biplanar fluoroscopy preferred
Vertebroplasty Technique
The following is a high-level summary. Full cement mixing protocols, pedicle access technique by spinal level, cement leak management algorithms, and kyphoplasty balloon inflation details are available in RadCall Pro.
Owl Eye Pedicle Entry
Patient prone on radiolucent table with biplanar fluoroscopy. On AP fluoroscopy, the pedicle appears as an oval shadow — the "owl eye." Position the trocar tip at the upper outer margin of the pedicle. Advance in the AP plane, keeping the tip within the pedicle oval. On AP view, the trocar should not cross the medial wall of the pedicle until it has entered the posterior vertebral body on lateral view. Advance to the anterior one-third of the vertebral body — tip should reach the anterior-middle junction on lateral.
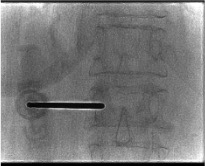
Cement Injection
Mix PMMA per manufacturer protocol. Wait for "toothpaste" consistency — test by aspirating into a 1 mL syringe; should flow slowly with resistance. Inject slowly under continuous biplanar fluoroscopy. Watch the lateral view primarily for posterior wall encroachment. Standard volumes: thoracic 2.5–4 mL, lumbar 6–8 mL per side.
STOP immediately at any posterior/epidural filling, foraminal leak, or venous runoff. Do not remove the needle — wait 1–2 minutes for the leading cement edge to polymerize and self-seal, then reassess. If posterior leak persists, reposition the needle more anteriorly. Never attempt to push through a posterior leak.
Kyphoplasty Technique
Key Differences from Vertebroplasty
Kyphoplasty uses a larger working cannula through bilateral pedicles. After pedicle entry, a hand-drill creates a working channel for the balloon. The balloon is advanced to the vertebral body and inflated incrementally under continuous lateral fluoroscopy to restore height before cement injection.
Balloon Inflation
Inflate slowly, pausing to check lateral fluoroscopy. Stop inflation immediately if: the balloon contacts the posterior cortex, pressure plateaus without further height gain, or end-plate breakthrough occurs. After target height or maximum resistance: fully deflate the balloon and remove before injecting cement.
Cement for Kyphoplasty
Use high-viscosity PMMA — unlike vertebroplasty, the cavity holds viscous cement without free flow through trabecular bone, significantly reducing extravasation risk. Fill the cavity from anterior to posterior. Inject promptly after balloon removal — the cavity can partially collapse if there is excessive delay.
Curved Balloon Kyphoplasty (AVAflex)
Single unipedicular access — the curved nitinol AVAflex stylet traverses midline into the contralateral hemivertebra, allowing bilateral cavity creation from a single access point. The curved balloon inflates to cover the entire vertebral body width. After deflation, the curved AVAflex needle enables targeted cement delivery across midline.
Complications
| Complication | Clinical Significance | Management |
|---|---|---|
| Epidural cement leak | Most feared — cord/cauda equina compression | Asymptomatic: close monitoring. Symptomatic new neurologic deficit → emergent spine surgery + CT |
| Foraminal leak | Radiculopathy (new back/leg pain) | Often self-resolves; rarely requires decompression |
| Venous/pulmonary CE | Asymptomatic PE in up to 5% on CT; symptomatic rare | Anticoagulation if hemodynamically significant; CT chest for hypoxia post-procedure |
| Intradiscal leak | Accelerates disc degeneration; adjacent fracture risk | Monitor; counsel on adjacent level fracture risk |
| Adjacent vertebral fracture | Altered biomechanics from stiffened cemented level | Counsel at discharge; return for new acute pain |
| Incomplete pain relief | 10–30% of patients | Re-evaluate: new fractures, alternate pain source, insufficient cement fill |
Post-Procedure Care
- Recover supine 1–2 hours; neurologic exam before discharge
- Ambulation typically possible day of procedure
- Pain relief timeline: Often immediate to 24–48h; transient pain increase first 24–72h (muscle spasm/inflammation) is common; near-complete improvement by 10–14 days in most patients
- Resume anticoagulation at 24 hours post-procedure (earlier if high thrombotic risk)
- Osteoporosis management referral — bisphosphonates, denosumab, or teriparatide; treating the underlying disease is critical to prevent cascade fractures
- Physical therapy for core strengthening and fall prevention; DEXA scan if not recently performed
- Counsel on adjacent fracture risk — return to ED for any new acute back pain or new neurologic symptoms
References
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. Chapters 16–17 (Vertebroplasty and Kyphoplasty).
- Wardlaw D, Cummings SR, Van Meirhaeghe J, et al. Efficacy and safety of balloon kyphoplasty compared with non-surgical care for vertebral compression fracture (FREE): a randomised controlled trial. Lancet. 2009;373(9668):1016–1024.
- Cazzato RL, Koch G, Garnon J, et al. Vertebral augmentation reduces all-cause mortality in non-neurologically impaired patients with osteoporotic vertebral fractures. Eur Radiol. 2021;31(3):1980–1989.
- Gangi A, Guth S, Imbert JP, et al. Percutaneous vertebroplasty: indications, technique, and results. Radiographics. 2003;23(2):e10.