Indications & Contraindications
Indications
- Penetrating or blunt extremity vascular injury with active hemorrhage, pseudoaneurysm, AV fistula, or vessel occlusion on CTA
- Hard signs (emergent): pulsatile bleeding, expanding hematoma, absent distal pulses, palpable thrill or bruit
- Soft signs (CTA then decide): diminished pulses, nerve deficit, proximity wound, history of hemorrhage now controlled
- Iatrogenic arterial injury (post-catheterization pseudoaneurysm, AV fistula)
- Delayed presentation of traumatic pseudoaneurysm
Contraindications
- Complete vessel transection with large gap requiring surgical repair — endovascular crossing may not be feasible
- Compartment syndrome requiring fasciotomy first — embolization does not fix compartment syndrome
- Signs of skin ischemia or necrosis — indication for surgery
- Compression of neurovascular bundle requiring surgical decompression
- Inadequate landing zones for stent-graft (no proximal/distal fixation site)
- Relative: vessel diameter <5 mm (limits stent-graft options), injury at high-flexion zone
Hard Signs vs. Soft Signs Triage
| Finding | Classification | Action |
|---|---|---|
| Pulsatile bleeding | Hard sign | Emergent OR / angio |
| Expanding hematoma | Hard sign | Emergent OR / angio |
| Absent distal pulses | Hard sign | Emergent OR / angio |
| Palpable thrill / bruit | Hard sign | Emergent OR / angio |
| Diminished pulses | Soft sign | CTA → decide |
| Nerve deficit adjacent to vessel | Soft sign | CTA → decide |
| Proximity wound (no other signs) | Soft sign | CTA → decide |
Pre-Procedure Planning
Imaging & Assessment
- CTA of affected extremity (arterial + delayed phases) — roadmap for angiographer; identifies injury type (extravasation, PSA, AV fistula, occlusion/dissection)
- CTA provides additional soft-tissue and osseous information critical for operative planning
- Be aware of anatomic variants (peronea arteria magna in up to 5% of population, persistent median artery in upper extremity)
Preparation & Consultation
- Tourniquet if active hemorrhage — temporizing measure until intervention
- Type & screen / crossmatch; activate MTP if hemodynamically unstable
- Ortho / vascular surgery consultation — multidisciplinary decision: endovascular vs. open repair
- Assess for compartment syndrome (tense compartment, pain with passive stretch, paresthesias)
- Hybrid OR preferred if available; allows conversion to open if needed
Relevant Anatomy
Upper Extremity
- Subclavian → Axillary → Brachial → Radial / Ulnar
- Profunda brachial artery — key collateral; can be safely embolized
- Radial or ulnar can be embolized individually if palmar arch intact (confirm with Allen test equivalent)
- Subclavian segment proximal to vertebral artery origin may be occludable if vertebrobasilar circulation intact
- At-risk nerves: brachial plexus (axillary/subclavian injuries), median nerve (brachial artery), ulnar nerve (ulnar artery)
- Internal mammary artery (IMA): key collateral in proximal subclavian/axillary occlusion — may reconstitute distal brachial via thoracoacromial and lateral thoracic arcade; preserve when possible during embolization
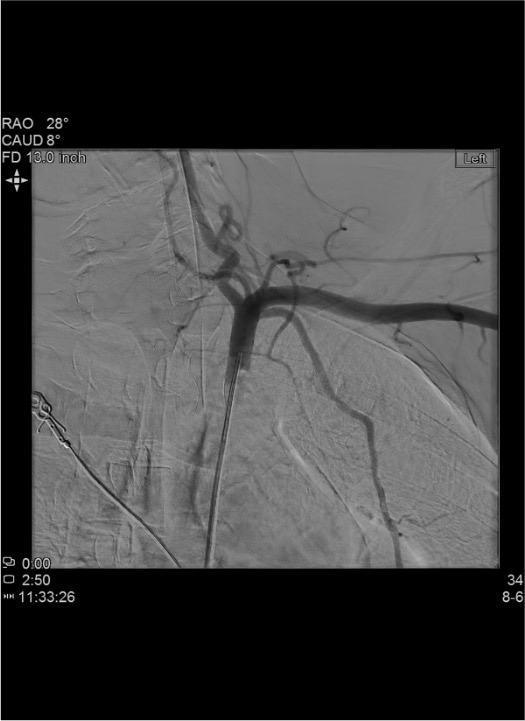
Lower Extremity
- CFA → SFA → Popliteal → Tibial trifurcation (anterior tibial, posterior tibial, peroneal)
- Profunda femoris — critical collateral pathway; Gelfoam embolization of main trunk only in life-threatening hemorrhage and only if SFA patent
- Geniculate arteries — collateral network around knee
- Trifurcation vessels: any one can be embolized individually, but at least one vessel must be maintained for foot perfusion
- At-risk nerves: sciatic/peroneal nerve (popliteal injuries), femoral nerve (inguinal/CFA region)
Embolization Safety by Vessel
| Vessel | Safe to Embolize? | Notes |
|---|---|---|
| Subclavian / Axillary | Usually not | Conduit vessels; consider covered stent |
| Brachial | Usually not | May consider if intact profunda brachial collaterals |
| Profunda brachial | Yes | Muscular branch; safe to sacrifice |
| Radial / Ulnar | Yes | Only after confirming intact palmar arch |
| CFA / SFA / Popliteal | No | Conduit vessels; stent-graft if injured |
| Profunda femoris | Usually not | Gelfoam only if life-threatening and SFA patent |
| Tibial trifurcation | Yes (individually) | Maintain at least one vessel for foot perfusion |
Technique
Vascular Access
- Contralateral femoral artery — most common; up-and-over for ipsilateral lower extremity injuries
- Ipsilateral femoral access — for proximal upper extremity or contralateral lower extremity injuries
- Radial access preferred for upper extremity injuries — contralateral radial or femoral approach; if ipsilateral radial needed (proximal radial/ulnar injury): confirm dual-hand supply with Allen test first; avoid brachial access if possible (>5F brachial sheath carries substantial thrombosis + median nerve injury risk)
- Transpedal retrograde access described for distal lower extremity injuries when femoral access not feasible
Equipment Considerations
- Coils (detachable preferred for precision; pushable for scaffolding)
- Gelfoam slurry or pledgets (temporary embolization, rapid deployment)
- Covered stent-grafts (Viabahn or similar; 5–10 mm diameters)
- Microcatheters (coaxial system for selective embolization)
- Balloon catheters (tamponade, PTA)
- Aspiration thrombectomy catheter (for distal embolization rescue)
Active Hemorrhage from Muscular Branch
Pseudoaneurysm (PSA)
Arteriovenous (AV) Fistula
Vessel Occlusion / Dissection
Community Cards
Landmarks & Identification
CTA Correlation
- Match CTA findings to angiographic anatomy: identify injury level relative to bony landmarks (humeral head for axillary, mid-shaft femur for SFA, knee joint line for popliteal)
- Fracture fragments and bullet/shrapnel trajectories on CTA predict vessel injury location
- Delayed-phase CTA images demonstrate PSA filling, AV fistula early venous opacification, and extent of extravasation
Pulse Points & Angiographic Identification
- Upper extremity: subclavian (supraclavicular), axillary (axilla), brachial (medial arm/antecubital fossa), radial (wrist)
- Lower extremity: femoral (inguinal crease), popliteal (popliteal fossa), dorsalis pedis, posterior tibial (medial malleolus)
- On angiogram: identify injury as extravasation (active bleed), contained PSA (delayed filling), intimal flap (linear lucency), or abrupt cutoff (occlusion)
- Run angiographic series through to venous phase to identify AV fistula (early venous opacification)
Troubleshooting
Guidewire Cannot Traverse Transected or Occluded Segment
Attempt hydrophilic wire with support catheter. Try different wire/catheter combinations. If gap is large or vessel completely transected, endovascular approach may not be feasible. Convert to surgical bypass or interposition graft. Consider dual-access (antegrade + retrograde with snaring) for short-gap transections. Distal transections with small gaps are more amenable to antegrade crossing.
Absent Distal Pulses After Stent Placement or Embolization
Check for distal embolization — perform runoff angiogram. If thrombus in distal bed: aspiration thrombectomy or catheter-directed thrombolysis. Assess for vasospasm (give intra-arterial vasodilator: nitroglycerin 100–200 mcg or verapamil 2.5–5 mg). Check compartment pressures — fasciotomy threshold (compartment pressure >30 mmHg or within 30 mmHg of diastolic). Stent-graft thrombosis: re-cross and PTA, consider thrombolysis.
More Than One Site of Vascular Injury Identified
Prioritize proximal injury (inflow) first, then address distal injuries. Complete angiographic survey of entire extremity before ending case. Coordinate with surgery for combined approach if endovascular repair addresses proximal injury and surgical repair addresses distal or vice versa. Consider overall ischemia time when planning multi-level intervention.
Inadequate Landing Zones or Vessel Size Mismatch
Measure vessel diameter on CTA and on-table angiogram. Stent-graft requires adequate healthy vessel proximal and distal to injury for fixation. If landing zones inadequate: consider surgical repair. Vessels <5 mm may not accommodate available covered stents. Self-expanding stents preferred in mobile areas (axillary, popliteal) to accommodate flexion.
Microcatheter Dislodges During Coil Deployment
Ensure stable coaxial system with guide catheter well-seated. Match coil diameter to vessel size to prevent displacement. Use detachable coils for precise placement; reposition before deployment if misplaced. Avoid oversized coils that can push the microcatheter out of position. If kick-out occurs and coil migrates distally, retrieve with snare if possible.
Complications
Intraprocedural / Early
- Distal embolization — most significant treatment-related complication; nontarget embolization of coils, thrombus, or plaque debris; frequent neurovascular exams critical in periprocedural period
- Access site complications — hematoma, pseudoaneurysm, AV fistula at puncture site; brachial access >5 Fr carries substantial thrombosis and median nerve compression risk — prefer radial or femoral approach whenever feasible
- Vessel perforation / dissection — from wire or catheter manipulation in traumatized vessel
- Stent malposition — covering critical side branches or failing to cover entire injury
Post-Procedural / Late
- Compartment syndrome — can develop or worsen after revascularization (reperfusion injury); monitor compartment pressures; fasciotomy if pressure >30 mmHg or within 30 mmHg of diastolic
- Amputation — limb loss from failed revascularization, irreversible ischemia, or uncontrolled hemorrhage
- Stent thrombosis — early or late; ensure antiplatelet therapy when trauma setting allows; duplex surveillance
- Nerve injury — from original trauma, compartment syndrome, or procedural manipulation
- Infection — stent-graft infection (rare); contaminated wound field increases risk
Pearls & Pitfalls
References & Resources
Key Concepts
- SIR 2020 consensus statement supports embolization of expendable extremity arteries; stent-grafts for conduit vessels
- Technical and clinical success rates for endovascular treatment of extremity arterial injuries: 80–100%
- Endovascular management associated with decreased operative time, blood loss, and iatrogenic injury vs. open repair
Primary References
- Weaver JJ, Chick JFB, Monroe EJ, Johnson GE. Life and Limb: Current Concepts in Endovascular Treatment of Extremity Trauma. Semin Intervent Radiol. 2021;38(1):64–74. DOI: 10.1055/s-0041-1724011
- Kuwahara JT, Kord A, Ray CE Jr. Penetrating extremity trauma: endovascular versus open repair? Semin Intervent Radiol. 2020;37(1):55–61.
- Feliciano DV, Moore FA, Moore EE, et al. Evaluation and management of peripheral vascular injury. Part 1. Western Trauma Association/Critical Decisions in Trauma. J Trauma. 2011;70(6):1551–1556.
- Reuben BC, Whitten MG, Sarfati M, Kraiss LW. Increasing use of endovascular therapy in acute arterial injuries: analysis of the National Trauma Data Bank. J Vasc Surg. 2007;46(6):1222–1226.
- SIR Consensus Statement on the Role of Endovascular Interventions for Trauma, 2020.