Indications & Contraindications
Indications
- Same spectrum as celiac plexus: pancreatic cancer pain, chronic pancreatitis, upper abdominal malignancy
- Preferred over celiac plexus when: distorted celiac anatomy from tumor encasement prevents safe retrocrural/anterocrural access
- Failed celiac plexus block — splanchnic approach targets the nerves proximal to the plexus
- Operator preference to avoid anterocrural approach near the aorta
- Splanchnic nerve ablation (RFA/cryo) offers more durable pain relief than chemical neurolysis in selected patients
Contraindications
- Coagulopathy (INR >1.5, platelets <50K)
- Inability to tolerate prone positioning
- Aortic aneurysm extending to T11–T12 level (proximity to target)
- Prior pneumothorax or compromised ipsilateral lung function (relative)
- Bowel or lung interposition in planned needle path
Splanchnic vs. Celiac Plexus: Key Comparison
| Feature | Celiac Plexus | Splanchnic Nerve |
|---|---|---|
| Target level | T12–L1 (anterolateral aorta) | T11–T12 paravertebral |
| Paralysis risk | <1% (anterior spinal artery proximity) | Lower (approach above aortic level) |
| Pneumothorax risk | Low | Higher (proximity to pleural space) |
| Distorted anatomy | Tumor encasement = higher risk | More accessible when celiac anatomy obscured |
| Ablation modality | Chemical (ethanol/phenol) or cryoneurolysis | RFA, cryoablation, or chemical |
Pre-Procedure Planning
Imaging Review
- CT chest and abdomen: identify T11–T12 paravertebral space, rib heads, pleural reflection, proximal lung parenchyma
- Plan bilateral posterolateral approach to T11–T12 paravertebral fat anterior to vertebral body
- Identify diaphragmatic attachment level — target is at or just above the diaphragmatic crus
- Assess for pleural adhesions, effusions, or prior pneumothorax (relative contraindication)
Labs & Patient Prep
- CBC, PT/INR (INR ≤1.5), platelets ≥50K
- IV access ×2; NPO 6h for moderate sedation / MAC
- 1 L NS IV pre-procedure (orthostatic hypotension prevention)
- Confirm ablation modality: RFA probe, cryoprobe, or 22G Chiba (chemical block)
- For RFA: confirm grounding pads available (not required for cryoablation or chemical)
Relevant Anatomy
Splanchnic Nerve Origins
- Greater splanchnic nerve: arises from T5–T9 sympathetic ganglia; carries preganglionic fibers from the thoracic sympathetic trunk
- Lesser splanchnic nerve: arises from T10–T11 sympathetic ganglia
- Least splanchnic nerve: arises from T12 sympathetic ganglion (inconstant)
- All three nerves converge caudally to form the celiac plexus at T12–L1
- Interrupting at T11–T12 blocks visceral pain transmission before the plexus is formed
Paravertebral Target Space
- Target: T11–T12 paravertebral fat space, anteromedial to the rib head, anterior to the vertebral body
- Nerves run in a groove between the vertebral body and the rib head at this level
- Needle tip should be in the paravertebral fat anterior to the rib head / costovertebral junction
- Diaphragmatic crus runs just caudal to this level; the splanchnic nerves cross under the crus to reach the celiac plexus
- Pleural reflection is immediately adjacent — monitor for apical spread of contrast or ice ball toward pleural space
Supplies & Setup
Chemical Block Setup
- 22G Chiba needles ×2 (15 cm)
- Extension tubing ×2
- Dilute iodinated contrast (30:1 saline:contrast) for test injection
- Bupivacaine 0.25% — 5–10 mL per side (block)
- Absolute ethanol 100% or phenol 6–10% — 5–10 mL per side (neurolysis)
- 10 mL syringes ×4
RFA / Cryoablation Setup
- RFA: 17–18G RFA probe (e.g., Cool-Tip or VIVA RF); grounding pads ×2; RF generator
- Cryoablation: 17G cryoprobe ×2 (one per side); argon/helium gas system
- RFA protocol: 80–90°C × 90 sec per probe position
- Cryoablation protocol: freeze–thaw–freeze cycle (2 × 8–10 min freezes, 5 min passive thaw)
- Standard sterile procedural tray, drapes, lidocaine 1%
Medications (Peri-procedure)
- IV fentanyl 50–100 mcg if chemical neurolysis planned
- Midazolam 1–2 mg IV for moderate sedation
- 1 L NS IV pre-procedure; continue at 100 mL/h during case
- Loperamide (Imodium) 2 mg PRN — discharge prescription
- Tylenol 975 mg PO q8h post-procedure for back pain
Procedure Steps
CT Planning at T11–T12
Prone Positioning & Sterile Prep
Probe / Needle Advancement to T11–T12 Paravertebral Space
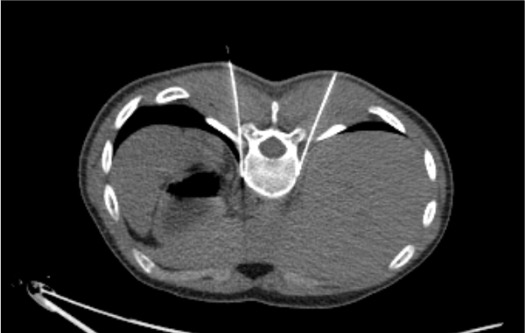
CT Confirmation of Probe Position
Test Injection (Chemical Technique) or Pre-ablation Check
Energy Delivery / Neurolytic Injection
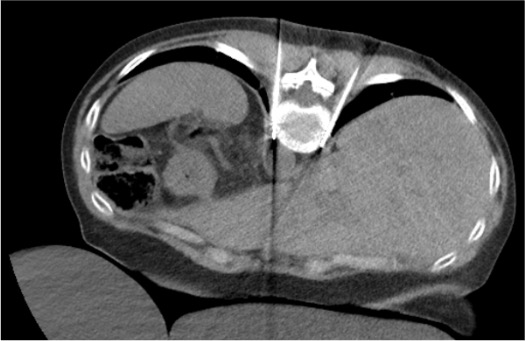
Post-ablation CT & Withdrawal
Community Cards
Troubleshooting
Probe Enters Pleural Space During Advancement
If CT shows probe has entered the pleural space, withdraw immediately to the chest wall. Do not inject any neurolytic agent with pleural access. Small pneumothorax from needle passage: observe, supplemental O2. If patient becomes symptomatic: pause procedure, determine pneumothorax size on CT. Small and asymptomatic: complete contralateral side and monitor. Large or symptomatic: place pigtail catheter before completing procedure.
Blood Aspirated from Probe or Hematoma Visible on CT
Intercostal neurovascular bundle runs along the inferior border of each rib. Advance probe above the rib (superior border) to avoid the bundle. If blood aspirated: withdraw to subcutaneous fat, apply pressure. Small hematoma usually self-limited. Monitor vitals. For expanding hematoma or active extravasation: IR arteriography and embolization of intercostal artery.
Probe Too Posterior or Too Lateral
Probe tip posterior to rib head will not reliably reach the splanchnic nerve. Advance tip under CT guidance to a position anterior to the costovertebral junction. For chemical technique, inadequate spread on test injection: reposition needle tip more anteriorly into the paravertebral fat and repeat test injection.
Cryoablation Ice Ball Extends Toward Pleural Space
Monitor ice ball continuously on CT during freeze cycles. If ice ball extends within 5 mm of pleural reflection: terminate freeze cycle, allow passive thaw, reposition probe 1–2 cm caudally, resume freeze. Do not allow ice ball to extend through pleural reflection — risk of pleural frostbite and pneumothorax.
Complications
Common / Expected Side Effects
- Orthostatic hypotension — same mechanism as celiac plexus; splanchnic sympathectomy; usually 24–48h duration; IV fluid, fall precautions
- Diarrhea — parasympathetic release from sympathetic denervation; loperamide PRN; typically 2–5 days
- Back and flank pain — post-procedure; related to needle access and local tissue response; Tylenol/NSAIDs
Serious Complications
- Pneumothorax — most feared; higher incidence than celiac plexus due to proximity of pleural space; post-procedure CT mandatory; treat symptomatically vs chest tube
- Intercostal neuralgia — injury to intercostal nerve during probe placement; burning pain in dermatome distribution; usually resolves weeks to months
- Retroperitoneal hematoma — from vessel injury; rare; monitor BP and hematocrit
- Paralysis: significantly lower risk than celiac plexus approach (approach is above the aorta and anterior spinal artery territory)
Post-Procedure Care & Pearls
Recovery
- Post-procedure CT before leaving the CT suite — mandatory to exclude pneumothorax
- BP monitoring q15 min × 2h; IV fluid continued
- Assisted first ambulation; fall precautions for orthostatic hypotension
- Discharge when BP stable and no pneumothorax on CT
- Pain response: expect improvement within 24–72h; reassess at 2 weeks
Discharge Instructions
- Rise slowly from supine/sitting for 3–5 days
- Loperamide 2 mg PRN for diarrhea
- Return precautions: shortness of breath, chest pain → ER immediately (late pneumothorax possible)
- Leg weakness or numbness → ER (rare somatic nerve involvement)
- Pain reassessment follow-up at 2 weeks
- Provide patient with pain diary for tracking daily pain levels before follow-up appointment.
Technique Pearls
References & Resources
Cryoneurolysis Literature
- Prologo JD, Zabala ZE (Chapter 12): CT-guided cryoneurolysis of involved nerve roots; two 8–10 min freeze cycles; important for motor nerve injury counseling
- Moussa AM, Santos E, Camacho JC (Chapter 13): cryoneurolysis without direct nerve involvement; intercostal cryoneurolysis; preliminary nerve block as predictive test
- Bittman RW et al. Percutaneous image-guided cryoneurolysis. AJR Am J Roentgenol. 2018;210(2):454–465.
Primary References
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. DOI: 10.1055/b000000387
- Nitschke AM, Ray CE Jr. Percutaneous neurolytic celiac plexus block. Semin Intervent Radiol. 2013;30(3):318–321.
- Prologo JD, Patel I, Buethe J, Bohnert N. Ablation zones and weight-bearing bones: points of caution for the palliative interventionalist. J Vasc Interv Radiol. 2014;25(5):769–775.