Indications & Patient Selection
Indications
- Lytic vertebral metastasis with pain — standard indication; VAS >4 despite opioids; primary tumors include RCC, breast, lung, thyroid
- Sclerotic vertebral metastasis — prostate, breast; RFA preferred (lytic lesions have lower impedance; sclerotic lesions respond to RFA through mechanical stabilization + ablation)
- Multiple myeloma with vertebral body compression fracture — bipolar RFA + kyphoplasty; RFA creates cavity effect for more predictable cement fill
- Spinal hemangioma — painful or aggressive; cementoplasty ± ablation
- Osteoid osteoma of spine — RFA curative (CT-guided thermal ablation of nidus); pedicle/posterior element location
- Radiation-resistant tumors (RCC, sarcoma) or radiation-naive patients refusing EBRT
- Post-SBRT local progression (with radiation oncology confirmation of max dose reached)
Contraindications
- Epidural tumor causing cord compression — surgical decompression first; ablation alone will not relieve osseous retropulsion
- >50% vertebral body collapse without augmentation plan (fracture risk post-ablation)
- SINS ≥13 (frank instability) — surgical stabilization required
- Posterior wall not intact with epidural tumor <5 mm from cord without thermal protection plan
- Cervical spine sclerotic lesions (avoid without credentialed spine surgeon backup)
- Active infection at proposed access site
- Life expectancy <3 months (relative; discuss with palliative care)
Patient Selection Criteria
- ECOG performance status 0–2 (Karnofsky ≥60); ECOG 3–4 requires careful multidisciplinary discussion
- Life expectancy ≥3 months for curative-intent procedures; palliative ablation can be considered for shorter survival if quality of life improvement expected
- Pain VAS ≥4 despite opioid analgesia; pain localized to treated level(s)
- ≤3 spinal levels per session (avoid excessive ablation zone in single anesthesia)
- SINS 0–6 (stable): ablation alone or with augmentation; SINS 7–12 (potentially unstable): multidisciplinary discussion, augmentation planned; SINS ≥13: surgical consult required
- Multidisciplinary tumor board for primary bone tumors and complex cases
Pre-Procedure Planning
Imaging Review
- Dedicated MRI spine with gadolinium — assess marrow replacement extent, epidural involvement, posterior wall integrity, cord distance
- CT for cortical integrity, pedicle width, posterior wall assessment, and transpedicular access planning; measure distance from probe to epidural space
- Bone scan (Tc-99m MDP) for tumor burden and additional sites not seen on MRI
- PET-CT for treatment response planning (metabolically active disease)
- Confirm: lesion is lytic vs. sclerotic vs. mixed (determines ablation modality preference)
- Confirm posterior vertebral wall intact; <5 mm epidural clearance = thermal protection required
Labs & Multidisciplinary
- CBC, CMP, coagulation; type and screen for augmentation cases
- Neurologic exam baseline: document motor strength, reflexes, sensory level
- Multidisciplinary tumor board for primary bone tumors (osteoid osteoma diagnosis required before RFA)
- Radiation oncology coordination: SBRT vs. ablation discussion; if prior SBRT → confirm max cord dose not exceeded; document radiation-induced fracture risk
- Spine surgery consultation if SINS ≥7 (potential instability)
- Anesthesia plan: general vs. MAC; motor/sensory evoked potential monitoring for complex cases near cord
Ablation Modality Selection
| Modality | Best For | Advantage | Limitation |
|---|---|---|---|
| RFA (navigational bipolar) | Lytic & sclerotic mets; osteoid osteoma; myeloma | Real-time thermocouple monitoring; no grounding pads; articulating electrode reaches central VB; creates cavity for cement | Ablation zone occult on CT; heat-sink from CSF/venous plexus |
| MWA | Larger lytic mets; osteoblastic lesions; near vasculature | Less heat-sink; works in sclerotic bone; no grounding pads; faster large zone | Zone less predictable; rapid high power → neural injury risk; tip artifact on CT |
| Cryoablation | Large soft tissue component; posterior elements; paravertebral extension; MRI-compatible cases | Ice ball visible in real time on CT; less intraprocedural pain; multiple probes for sculpted zone | No visualization in osteoblastic lesions; longer procedure; delay cement by 30–60 min post-thaw |
Anatomy & Safety Considerations
Critical Anatomic Zones
- Posterior vertebral body wall — most critical boundary; intact cortex does NOT prevent thermal energy propagation (all modalities)
- Epidural space — target safety margin: ≥1 cm from spinal cord; 5–10 mm = thermal protection required; <5 mm = high risk, reconsider approach
- Pedicles — transpedicular access; avoid medial wall breach → epidural space; pedicle width determines cannula size
- Neuroforamina — exiting nerve roots at each level; foraminal thermal spread causes radiculopathy
- Heat-sink effect: posterior vertebral body and pedicles benefit from CSF/venous plexus cooling — limits posterior cord injury but also limits ablation efficacy posteriorly
Thermal Protection Techniques
- Epidural cold saline hydrodissection: epidural catheter → cold D5W (ionic solutions conduct electricity, avoid with RFA) → active cooling during ablation; initiate when epidural temperature reaches 45°C (heat) or 10°C (cryo)
- CO2 pneumodissection: inject CO2 into epidural space or neuroforamina → insulating gas layer prevents thermal conduction to cord; monitor volume to avoid cord compression
- Thermocouple monitoring: temperature probes in epidural space and/or foramina → real-time feedback; pause ablation if temp exceeds 45°C (heat) or falls below 10°C (cryo)
- Neurophysiology monitoring: motor/somatosensory evoked potentials (MEPs/SSEPs) for cord-adjacent procedures; changes = stop ablation
- Patient feedback (moderate sedation): maintain consciousness during ablation to detect radiculopathy; patient reports = stop and assess
Technique
Ablation + Augmentation Combined Technique
Positioning, Anesthesia & Setup
Pre-Procedure Medications
CT/Fluoroscopy Planning
Transpedicular Access
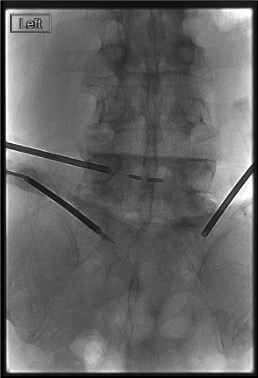
Thermal Protection Setup (if <1 cm Epidural Clearance)
Ablation
MWA: Advance MWA antenna(e) to target. Activate per manufacturer protocol (typically 45–65W, 10–15 min). Monitor for breakthrough pain or patient response.
Cryoablation: Advance cryoprobes. Freeze 10 min → active thaw 5 min → freeze 10 min. Monitor ice ball on CT in real time. Ice ball must remain ≥5 mm from posterior wall and epidural space.
Intraprocedural Assessment
Vertebral Augmentation (if Indicated)
Post-Procedure CT
Community Cards
Troubleshooting
Sclerotic Bone — Difficult Cannula Advancement
Sclerotic bone is dense and difficult to traverse. Use mallet for cannula advancement under fluoroscopy. If bone too sclerotic for standard cannula: curved or drill-assisted access systems. Confirm pedicle wall integrity with AP fluoroscopy before advancing to prevent medial breach into epidural space. RFA preferred for sclerotic lesions (effective in dense bone at lower power than MWA).
Probe Near Cord / Inadequate Epidural Clearance
CT confirms probe tip or ablation zone margin <5 mm from posterior wall or epidural space. Add active thermal protection immediately: initiate cold D5W epidural drip + CO2 pneumodissection. Place thermocouple for real-time monitoring. Reduce ablation power/time and ablate in shorter pulses. If unable to safely maintain ≥5 mm margin: abort ablation and discuss with spine surgery before proceeding.
Inadequate Ablation Zone Coverage
Post-ablation CT shows margin not encompassing tumor (especially posterior margin). Reposition electrode/antenna and ablate additional zone targeting undermargined area. For RFA: medial tip articulation achieves coalescent zones without additional access. For large tumors (>3 cm): planned overlapping zone strategy (front-to-back, then back-to-front) before starting.
Cement Leak on Fluoroscopy
Stop cement injection immediately. Small epidural leak: monitor closely; CT confirmation; neurology consultation for any new symptoms. Posterior wall leak with epidural cement: urgent CT; neurosurgery consultation; steroid (methylprednisolone 1 mg/kg IV) if cord compression suspected. Venous leak: usually self-limiting; monitor for pulmonary cement embolism.
Nerve Root Pain During Ablation (MAC Cases)
Patient reports burning, shooting leg pain during ablation = nerve root thermal injury signal. Stop ablation immediately. Assess dermatomal distribution. Add thermal protection (epidural cooling + CO2). If symptoms persist: abort ablation at this level; obtain CT to assess proximity. Transforaminal steroid injection post-procedure may provide relief for thermal radiculitis.
Complications
Major Complications
- Neurologic injury (spinal cord / nerve root) — most critical; most transient (radiculopathy, paresthesia); rare permanent deficit; epidural steroid + long-acting local anesthetic for transient cases; neurosurgery for worsening or progressive deficits
- Spinal cord infarct — rare; vascular injury or cement compression of radicular artery; immediate MRI; high-dose steroids; ICU
- Cement epidural leak with cord compression — emergent neurosurgery consultation; consider decompressive laminectomy
- Ablation-related pathologic fracture — weakened bone post-ablation; prevent with concurrent augmentation in weight-bearing segments
Minor / Expected Complications
- Post-ablation pain flare — common day 1–3; inflammatory response; dexamethasone 4 mg q8h × 3 days + scheduled NSAIDs + opioid PRN
- Radiculopathy (transient thermal radiculitis) — foraminal spread; transforaminal steroid injection; gabapentin
- Radiation recall with prior SBRT — ablation adjacent to SBRT field can trigger recall reaction; discuss with radiation oncology pre-procedure; steroid prophylaxis recommended
- Infection / discitis / osteomyelitis — rare; standard procedural asepsis; cefazolin prophylaxis for augmentation
- Cement pulmonary embolism — venous extravasation; usually asymptomatic; supportive; anticoagulation if symptomatic
- Skin thermal injury — monopolar RFA grounding pad burns; bipolar systems minimize this risk
Post-Procedure Care
Day 0 — Immediate Recovery
- Neurologic checks every 4 h for 24 h: motor strength (bilateral lower extremities), sensation, bowel/bladder function
- Pain management: ketorolac + acetaminophen scheduled; opioids PRN; PCA if severe post-ablation pain
- Dexamethasone 4 mg IV q8h × 24 h (post-ablation edema prophylaxis); then taper over 3–5 days
- Post-ablation pain flare expected: max day 1–2; typically resolves by day 3
- Maintain ambulation precautions if neurologic deficit noted
- Overnight monitoring standard; consider 2-night stay for cord-adjacent procedures
Days 1–7: Post-Ablation Syndrome
- Local pain, fever (up to 38.5°C), fatigue — expected and self-limiting
- Continue scheduled acetaminophen; taper ketorolac by day 5
- Pain diary documentation; VAS score at 24 h, 72 h, 1 week
- Significant pain improvement expected by 72 h in most patients (70–80% of lytic metastasis cases)
- Fever >38.5°C beyond 72 h: blood cultures, CT to exclude infection
- Patient education: call if new numbness, leg weakness, bowel/bladder changes, or uncontrolled pain
Imaging Follow-up Schedule
| Timepoint | Study | What to Assess |
|---|---|---|
| Immediately post-procedure | CT (same session) | Ablation zone, cement distribution, epidural space, acute neural compression |
| 6–8 weeks | MRI spine with gadolinium | Local tumor control: non-enhancing ablation zone = adequate; enhancing nodule at margin = residual/recurrence |
| 3 months | MRI spine | Tumor control assessment; new lesions; osteoid osteoma — symptom resolution = curative |
| 6 months | MRI ± bone scan | Continued surveillance; assess new metastatic disease; cement integration |
Pearls & Pitfalls
Technique Pearls
Critical Pitfalls
References & Resources
Modality Comparison for Spinal Lesions
| Feature | RFA (Navigational Bipolar) | MWA | Cryoablation |
|---|---|---|---|
| Ablation zone visibility on CT | Occult (use thermocouples) | Poorly visible (tip artifact) | Excellent (ice ball = low density) |
| Sclerotic bone efficacy | Good (low power, predictable) | Good (less impedance-sensitive) | Poor (ice ball occult in sclerotic) |
| Lytic bone efficacy | Excellent | Excellent (less heat-sink) | Excellent |
| Soft tissue / paravertebral component | Limited reach | Moderate | Excellent (sculpted zones) |
| Intraprocedural pain | Moderate | High | Low |
| Heat-sink effect | Yes (CSF/venous plexus) | Less susceptible | N/A (cold) |
| Grounding pads needed | No (bipolar) | No | No |
| Metallic implants concern | Low (bipolar) | None | None |
| Cement timing after ablation | Immediate | Immediate | Delay 30–60 min (thaw) |
| Best indication | Lytic & sclerotic mets; myeloma; osteoid osteoma | Large lytic; osteoblastic; near vasculature | Large soft tissue component; posterior elements; paravertebral |
Primary References
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. DOI: 10.1055/b000000387
- Tomasian A, Jennings JW. Percutaneous vertebral augmentation. Semin Intervent Radiol. 2019;36(4):256–263.
- Tomasian A, Gangi A, Wallace AN, Jennings JW. Percutaneous thermal ablation of spinal metastases: recent advances and review. AJR Am J Roentgenol. 2018;210(1):142–152.
- Tran DQ, et al. Cryoneurolysis. Reg Anesth Pain Med. 2021;46(3):255–263.
- Wallace AN, et al. The metastatic spine disease multidisciplinary working group algorithms. Oncologist. 2015;20(10):1205–1215.
- Shah LM, Jennings JW, et al. ACR Appropriateness Criteria: management of vertebral compression fractures. J Am Coll Radiol. 2018;15(11S):S347–S364.
References & Resources
Key Guidelines
- SIR Standards of Practice for Thermal Ablation
- CIRSE Standards for Spine Ablation
- NCCN Bone Cancer Guidelines
Primary References
- Prologo JD et al. Percutaneous CT-guided cryoablation of the celiac plexus vs. the splanchnic nerves. J Vasc Interv Radiol. 2015;26(11):1639-1647.e1.
- Callstrom MR et al. Painful metastases involving bone: percutaneous image-guided cryoablation — prospective trial. Radiology. 2006;241(2):572-580.
- Gangi A et al. Interventional radiologic procedures with CT guidance in cancer pain management. Radiographics. 1996;16(6):1289-1304.