Indications & Patient Selection
Indications
- Pudendal neuralgia — chronic perineal pain (perineum, labia/scrotum, penis, anorectal region)
- Pain worse with sitting, better standing or lying
- Burning, electric shock quality, or hypersensitivity in pudendal distribution
- Entrapment at Alcock’s canal (by sacrospinous ligament, between sacrotuberous and sacrospinous ligaments)
- Post-surgical pudendal neuropathy (hernia repair, pelvic surgery)
- Post-radiation or childbirth injury to pudendal nerve
- Oncologic pain in pudendal distribution (vulvar, penile, rectal malignancy)
- Diagnostic block (Nantes criterion 5) before proceeding to ablation
- Cryoablation for refractory cases after positive diagnostic block
Contraindications
- Uncorrectable coagulopathy
- Active pelvic infection / gluteal abscess
- Pregnancy
- Negative diagnostic block (cryoablation unlikely to help)
- Structural cause not excluded (endometriosis, pelvic tumor, Tarlov cyst) — treat underlying cause first
Nantes Criteria for Pudendal Nerve Entrapment (All 5 Required)
| # | Criterion | Notes |
|---|---|---|
| 1 | Pain in the territory of the pudendal nerve | Perineum, anorectal, genitalia |
| 2 | Pain worsened by sitting | Key feature; relief standing or lying |
| 3 | Patient not woken by pain at night | Distinguishes from central sensitization |
| 4 | No objective sensory loss on examination | Objective loss suggests structural nerve damage |
| 5 | Positive diagnostic pudendal nerve block | ≥50% pain reduction lasting ≥24 h = positive |
Block vs. Cryoablation Decision
- Diagnostic/therapeutic block: first-line; local anesthetic ± steroid; positive block = ≥50% pain reduction for ≥24 h
- Repeat therapeutic block: up to 3–4 per year; avoid repeat same nerve injection within 4–6 weeks
- Cryoablation: indicated after definite positive block(s) in refractory disease; superior to chemical neurolysis for benign pain (reversible, lower dysesthesia risk)
- Pulsed RFA: alternative for ablation of this mixed motor/sensory nerve (42°C × 120 s) — preferred over continuous RFA to limit motor fiber injury
Pre-Procedure Planning
Imaging
- MRI pelvis (rule out structural cause: endometriosis, pelvic tumor, Tarlov cyst, pelvic floor dysfunction)
- MR neurography if available — increased T2 signal in pudendal nerve = inflammation/entrapment
- CT for procedural planning — visualize ischial spine, sacrospinous ligament, and pudendal canal geometry
- Review prior pelvic surgery operative notes for relevant anatomy distortion
Labs & Assessment
- INR, platelet count (SIR Cat 1 — thresholds: INR ≤2.5, plt ≥25K)
- Pudendal nerve terminal motor latency (PNTML) testing if available — abnormal (>2.2 ms) supports entrapment
- Baseline VAS pain score — document standing vs. sitting
- Prior pain management history: PT, pelvic floor therapy, prior blocks, medications
- Anesthesia consult if MAC planned (cryoablation cases)
Anatomy
Nerve Course
- Origin: ventral rami of S2–S4 nerve roots (mixed motor and sensory)
- Exits pelvis through greater sciatic foramen, below piriformis muscle
- Crosses ischial spine; enters perineum via lesser sciatic foramen
- Travels through Alcock’s canal (pudendal canal): between medial surface of obturator internus (lateral) and ischiorectal fat (medial), under the obturator fascia
- Entrapment most common between sacrospinous and sacrotuberous ligaments at ischial spine
Terminal Branches
- Inferior rectal nerve — cutaneous innervation of external anal sphincter and perianal skin
- Perineal nerve — superficial branch: posterior scrotal/labial skin; deep branch (muscular): bulbospongiosus, ischiocavernosus, external urethral sphincter
- Dorsal nerve of penis / clitoris — sensory innervation
CT Landmarks for Targeting
- Primary target (Alcock’s canal approach): medial border of obturator internus muscle in the pudendal canal — nerve runs as posterior-most structure of the neurovascular bundle; intermediate density compared to adjacent vessels
- Alternative target (ischial spine approach): nerve located between sacrospinous and sacrotuberous ligaments where they converge at ischial spine; injectate distributes anteromedially into Alcock’s canal
- Dual-site targeting: both ischial spine AND Alcock’s canal in same session increases block effectiveness
- Pudendal artery and vein run adjacent — aspirate before injection; always confirm no vascular opacification with dilute contrast
- Rectum lies medial — CT confirms needle tip position prior to injection
Technique
CT-Guided Block at Ischial Spine / Alcock’s Canal
Positioning & CT Planning
Skin Prep, Local Anesthesia
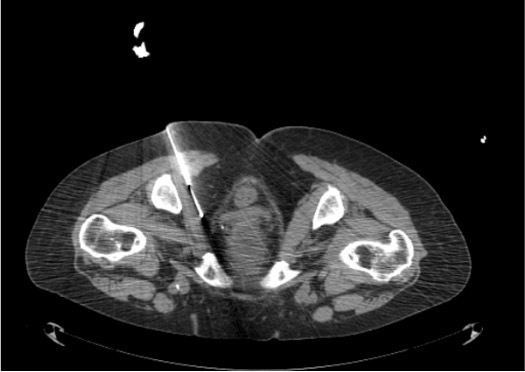
Needle Advancement
CT Confirmation of Needle Position
Aspiration + Contrast Injection
Medication Injection (Block)
Bilateral Injection (if Indicated)
Cryoablation Variant (After Positive Diagnostic Block)
Probe Placement
Freeze-Thaw Cycles
Ice Ball Monitoring
Active Thaw & Probe Removal
Community Cards
Troubleshooting
Intravascular Injection
Aspiration of blood OR rapid contrast washout on CT injection test → do not inject medication. Withdraw needle 2–3 mm, reposition medially, repeat aspiration and contrast test before injecting.
Rectal Wall Proximity
CT confirms needle tip or cryoprobe approaching rectal wall (<5 mm clearance). Redirect needle laterally. For cryoablation: if ice ball tracking toward rectum during freeze, active thaw and reposition probe before resuming. Air injection into perirectal fat (pneumodissection) can create protective buffer.
Inadequate Perineural Spread on Contrast
Contrast pools locally without tracking along canal — suggest fibrous entrapment or incorrect plane. Add hyaluronidase 100 units to injectate to dissolve fibrosis if suspected post-surgical scar. Alternatively, target both ischial spine AND Alcock’s canal to improve coverage.
Ice Ball Not Encompassing Nerve
CT demonstrates ice ball offset from target nerve. Active thaw, reposition probe 2–3 mm closer to nerve fascicles, resume freeze. Two probes placed in parallel 1 cm apart can be used for larger ablation zone if single probe insufficient.
Complications
Expected / Acceptable Effects
- Temporary perianal and perineal numbness — expected with any block; resolves 4–12 h after local anesthetic; may persist weeks after cryoablation
- Temporary urinary retention — advise patient to void before procedure; monitor ≥1 h post-block; Foley if unable to void
- Vaginal/scrotal numbness — expected and desired effect for pain control
- Mild gluteal soreness at probe insertion site (cryoablation)
Complications
- Rectal injury — rare; full-thickness injury requires surgical consultation; most rectal proximity issues resolve without treatment
- Gluteal hematoma — most self-limited; serial CT if expanding
- Pudendal arteriovenous fistula — rare post-cryoablation complication (reported); presents as pulsatile hematoma; CT angiography; endovascular treatment
- Infection / gluteal abscess — rare; antibiotics; CT-guided drainage if organized
- Sciatic nerve inadvertent block — if needle too lateral; transient foot weakness; resolves with local anesthetic metabolism
Post-Procedure Care
Immediate Recovery (Block)
- Observe 1–2 h post-procedure; confirm ability to ambulate safely
- Perianal sensory exam (light touch) to confirm expected sensory change in pudendal distribution
- Sitting test: assess pain level with sitting post-block — immediate improvement supports pudendal origin
- Voiding trial before discharge; Foley if urinary retention (>600 mL on bladder scan)
- No driving for 24–48 h (motor block risk); arrange driver
Recovery (Cryoablation)
- Observe 2–4 h; vital signs monitoring
- Expect perineal numbness for days to weeks — counsel patient this is expected
- Nerve regeneration begins 1–2 mm/day; full motor/sensory recovery 6–8 weeks (epineurium preserved)
- NSAIDs (ibuprofen 600 mg TID × 5 days) to manage post-cryoablation inflammation
- CBC not routinely required unless hematoma concern
Follow-up Schedule
| Timepoint | Assessment | Action |
|---|---|---|
| 24–48 h | Phone check (block cases) | Document pain score; confirm no urinary retention |
| 2 weeks | Clinic visit — pain reassessment, sensory exam | VAS score vs. baseline; document sitting vs. standing; repeat block if partial response |
| 6 weeks | Cryoablation follow-up | Assess motor/sensory recovery; pain diary review |
| 3 months | Outcome assessment | If pain returns: repeat cryoablation safe (epineurium intact = nerve can regenerate and be retreated) |
Pearls & Pitfalls
Technique Pearls
Critical Pitfalls
References & Resources
Primary References
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. DOI: 10.1055/b000000387
- Tran DQ, et al. Cryoneurolysis: a scoping review of the evidence. Reg Anesth Pain Med. 2021;46(3):255–263.
- Labat JJ, et al. Diagnostic criteria for pudendal neuralgia by pudendal nerve entrapment (Nantes criteria). Neurourol Urodyn. 2008;27(4):306–310.
- Prologo JD, et al. Percutaneous CT-guided cryoablation for the treatment of refractory pudendal neuralgia. Skeletal Radiol. 2015;44(5):709–714.
- Kastler A, et al. Dual site pudendal nerve infiltration: more than just a diagnostic test? Pain Physician. 2018;21(1):83–90.
References & Resources
Key Guidelines
- ASRA Practice Guidelines for Regional Anesthesia
- International Pudendal Nerve Entrapment Society Guidelines
Primary References
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology. Thieme; 2024.
- Benson JT, Griffis K. Pudendal neuralgia, a severe pain syndrome. Am J Obstet Gynecol. 2005;192(5):1663-1668.
- Labat JJ et al. Diagnostic criteria for pudendal neuralgia by pudendal nerve entrapment (Nantes criteria). Neurourol Urodyn. 2008;27(4):306-310.