Indications & Patient Selection
Indications
- Peripheral neuropathy — nerve entrapment syndromes causing focal pain or numbness
- Oncologic nerve pain — tumor invasion or compression of peripheral nerves
- Post-surgical neuropathy — scar entrapment following hernia repair, hip or groin surgery
- Diagnostic block — lidocaine 1–2 mL confirms nerve as pain source (≥50% relief) before ablation or definitive treatment
- Therapeutic block — bupivacaine + corticosteroid for medium-term relief
- Neurolysis — absolute ethanol (2–5 mL) for oncologic or refractory neuropathic pain after positive diagnostic block
Workup & Selection
- CT or MRI to identify nerve anatomy, mass lesions, and prior surgical anatomy before intervention
- EMG / NCS for entrapment confirmation — helps localize the affected segment
- MR neurography (3T) for complex or post-surgical cases with distorted anatomy — order before CT-guided intervention
- Failed conservative management (≥6 weeks) typically required before interventional approach
- Contraindications: Active infection at needle path · Uncorrectable coagulopathy · Allergy to injectate components · Absent diagnostic block confirmation before neurolysis
Common Nerve Targets
| Nerve | Syndrome | Symptoms |
|---|---|---|
| Lateral Femoral Cutaneous (LFCN) | Meralgia paresthetica | Lateral thigh numbness / burning |
| Genitofemoral (GFN) | Inguinal / scrotal pain | Groin / inner thigh pain post-hernia repair |
| Iliohypogastric / Ilioinguinal | Post-hernia pain | Lower abdominal / inguinal pain |
| Femoral | Femoral neuropathy | Anterior thigh pain / weakness |
| Obturator | Hip / medial thigh pain | Groin pain |
| Posterior Femoral Cutaneous (PFCN) | Sitting / perineal pain | Posterior thigh / perineum |
| Superior Gluteal | Piriformis syndrome | Buttock pain radiating down leg |
| Cluneal Nerves | Posterior iliac crest pain | Low back / buttock pain |
Pre-Procedure Checklist
Anatomy by Nerve
Lateral Femoral Cutaneous Nerve (LFCN)
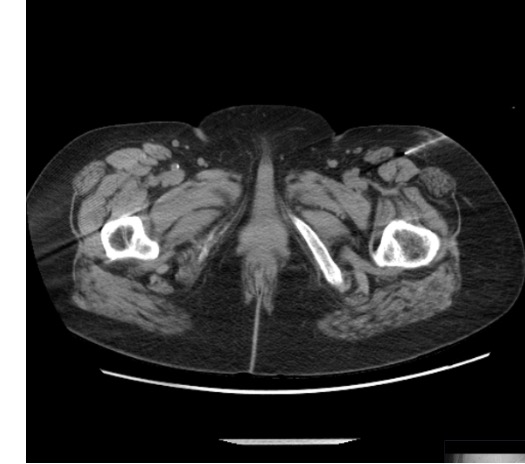
- Arises from L2–L3 nerve roots; purely sensory nerve
- Exits pelvis under inguinal ligament medial to ASIS; runs superficial to tensor fascia lata into the thigh
- Target: 1 cm medial and 1 cm inferior to ASIS — where nerve exits into thigh between fascia layers
- Approach: CT or US; supine or prone; 22G needle
- Syndrome: meralgia paresthetica — lateral thigh burning/numbness
Genitofemoral Nerve (GFN)
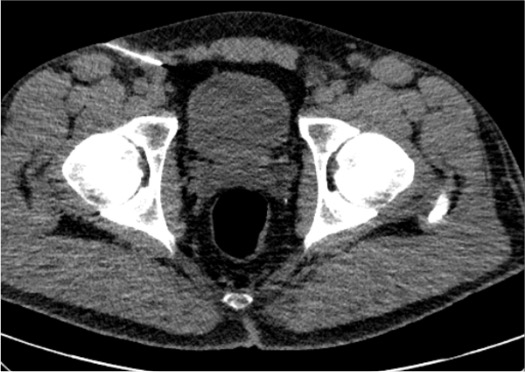
- Arises from L1–L2; runs on anterior surface of psoas muscle
- Divides into femoral branch (anterior thigh) and genital branch (scrotum/labia)
- Target: CT-guided; anterior to psoas at L3–L4 level (medial to iliopsoas, lateral to ureter)
- Approach: CT supine or lateral decubitus; 22G Chiba needle; lateral retroperitoneal approach
- Syndrome: groin/scrotal pain post-hernia repair
Iliohypogastric / Ilioinguinal Nerve
- Both arise from L1; run between transversus abdominis and internal oblique muscles
- Exit inguinal canal; innervate lower abdominal wall and inguinal region
- Target: between muscle layers at ASIS level; US or CT guidance
- Approach: in-plane US or CT axial at ASIS; transverse plane injection into fascial plane
- Syndrome: post-hernia repair lower abdominal/inguinal pain
Obturator Nerve
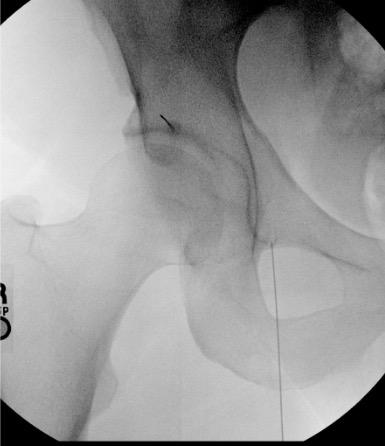
- Arises from L2–L4; exits pelvis through obturator foramen
- Divides into anterior branch (hip adductors, medial thigh sensation) and posterior branch
- Target: CT-guided; obturator foramen or medial to femoral vessels
- Approach: CT supine; coronal plane most useful; 22G needle
- Motor risk: adductor weakness — counsel about driving
Posterior Femoral Cutaneous Nerve (PFCN)
- Arises from S1–S3; exits greater sciatic foramen inferior to piriformis
- Runs deep to gluteus maximus; innervates posterior thigh and perineum
- Target: CT subgluteal approach; prone positioning
- Syndrome: sitting-related perineal/posterior thigh pain
Cluneal Nerves (Superior)
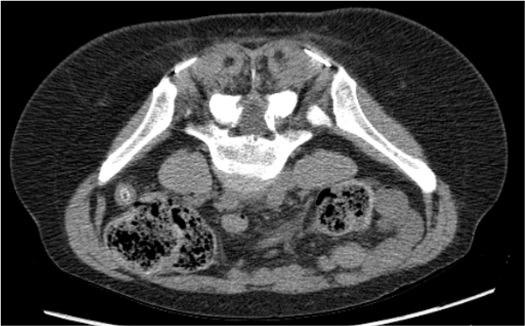
- Cross posterior iliac crest approximately 7 cm lateral to midline
- Innervate low back, buttock, and posterior iliac crest region
- Target: CT posterior approach at posterior iliac crest; prone positioning
- Syndrome: posterior iliac crest / low back pain, sometimes confused with SI joint pain
Technique
Default RadCall approach · share your own below
Supplies
Steps
CT planning
Position + skin prep
Advance 22G needle to target
Contrast injection
Inject medication
CT confirm and withdraw
Steps
CT planning — identify psoas margin
Lateral retroperitoneal approach
Contrast to confirm psoas fascia
Inject medication
CT Landmarks
Nerve Target Reference
| Nerve | CT Target | Best CT Plane | Key Anatomy |
|---|---|---|---|
| LFCN | Medial-inferior to ASIS; deep to inguinal ligament | Axial | Between fascia iliaca and tensor fascia lata |
| GFN | Anterior psoas surface at L3–L4 level | Axial | Medial to iliopsoas; lateral to ureter |
| Iliohypogastric / Ilioinguinal | Between transversus abdominis and internal oblique at ASIS | Axial at ASIS level | Fascial plane between muscle layers |
| Obturator | Obturator foramen; medial to femoral vessels | Coronal (most useful) | Anterior / posterior division at foramen |
| PFCN | Inferior to piriformis at greater sciatic foramen | Axial prone | Deep to gluteus maximus |
| Cluneal (superior) | Posterior iliac crest ~7 cm lateral to midline | Axial / coronal prone | CT posterior approach; subcutaneous at crest |
Fascial Plane Confirmation
- Contrast should track along the fascial plane containing the nerve — linear spread confirms perineural delivery
- Diffuse spread → too much volume injected; increases non-target effects
- Vascular filling (branching vessels opacify rapidly) → withdraw 2 mm, recheck before injecting
- Intraperitoneal spread (GFN) → withdraw; needle too deep; confirm retroperitoneal position before reinjecting
Positioning Tips
- LFCN / GFN / Obturator / Iliohypogastric: Supine — standard CT table positioning
- PFCN / Cluneal / Superior gluteal: Prone — place foam bolster under pelvis to flatten gluteal contour and open posterior approach
- Confirm target slice on CT scout before prepping and draping
- Mark skin entry point with CT-compatible marker before sterile prep
Troubleshooting
Intravascular contrast uptake on test injection
Likely cause: Needle tip in periforaminal vessel, retroperitoneal vessel, or fascial plane vasculature. Uncommon with 22G needle but always check before injecting medication.
Next step: Withdraw needle 2 mm, aspirate, reposition. Repeat contrast injection before any medication. Arterial or venous injury is extremely rare with 22G; manual pressure for 5 minutes if concern. Never inject medication — especially ethanol — with active vascular uptake.
Cannot identify small nerve on CT
Likely cause: Small nerve caliber (LFCN, ilioinguinal are 1–3 mm); post-surgical distortion; insufficient soft tissue contrast.
Next step: Use nerve anatomy landmarks (fascial planes) rather than attempting direct nerve visualization — target the fascial compartment containing the nerve. Consider ordering 3T MR neurography before procedure for precise anatomic mapping in post-surgical or complex cases.
Inadequate pain relief after block
Likely cause: Incomplete perineural spread (small volume, fascial plane missed); contributing nerve not targeted; incorrect nerve identified as pain source.
Next step: Consider slightly higher volume to ensure perineural spread (max 2–3 mL). Reassess whether an alternative contributing nerve is present (e.g., obturator and LFCN both contributing to thigh pain). Revisit EMG/NCS data and imaging.
Pain returns quickly after initial relief
Likely cause: Short duration of local anesthetic with early washout; underlying ongoing nerve irritation; structural cause not addressed.
Next step: Consider longer-acting agent (bupivacaine vs. lidocaine). If relief was ≥50% even briefly — positive diagnostic result; proceed to neurolysis (absolute ethanol), cryoablation, or radiofrequency ablation for durable relief.
Intraperitoneal spread on GFN block
Likely cause: Needle advanced too far anteromedially beyond retroperitoneal fat; peritoneum entered.
Next step: Withdraw needle; re-confirm on CT that tip is in retroperitoneal fat anterior to psoas before reinjecting. Intraperitoneal injection of a small amount of local anesthetic is not dangerous, but the block will be ineffective. Monitor for peritoneal signs briefly before discharging.
Complications
Immediate / Periprocedural
- Intravascular injection: Rare with 22G needle. Always aspirate before injecting; use contrast test dose under CT fluoroscopy. No epinephrine in block mixture. Absolute ethanol intravascular injection is catastrophic — confirm negative aspiration and fascial spread before neurolysis.
- Local anesthetic systemic toxicity (LAST): Use minimal effective dose; maximum bupivacaine 2 mg/kg. Symptoms: tinnitus, metallic taste, perioral numbness, seizure. Have resuscitation available. Lipid emulsion rescue for severe LAST.
- Temporary motor block: Genitofemoral / obturator blocks → adductor or thigh weakness. Counsel patient before procedure — no driving until resolved (typically 4–6 hours).
- Non-target spread: Large-volume LFCN or GFN block → femoral nerve involvement → anterior thigh weakness. Use minimal volumes (1–2 mL) to prevent this.
Delayed
- Infection: Rare with sterile technique (<0.1%). Fever and progressive pain post-procedure → CT with contrast; broad-spectrum antibiotics if soft tissue infection identified.
- Hematoma: Apply compression after procedure; monitor for expanding hematoma especially with anticoagulated patients. Usually self-limited.
- Neurolysis complications (ethanol): Permanent motor deficit, dysesthesia, deafferentation pain. Perform diagnostic block first — always. Hydrodissect nerve from adjacent structures (5–10 mL saline) before ethanol injection to protect skin, vessels, and bowel.
- Corticosteroid effects: Transient glucose elevation in diabetics; limit steroid injections per region per year. Not a routine concern for peripheral nerve blocks given small volumes used.
Critical Pearls
References
Citations
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. Ch. 31 (Pezeshk P, Wadhwa V, Chhabra A).
- Chhabra A, Andreisek G, Soldatos T, et al. MR neurography: past, present, and future. AJR Am J Roentgenol. 2011;197(3):583–591.
- Chhabra A, Soldatos T, Subhawong TK, et al. The application of three-dimensional diffusion-weighted PSIF technique in peripheral nerve imaging of the distal extremities. J Magn Reson Imaging. 2011;34(4):962–967.
- Chhabra A, Faridian-Aragh N, Chalian M, et al. High-resolution 3T MR neurography of the lumbosacral plexus. Radiographics. 2012;32(3):967–983.
- SIR Standards of Practice Committee. Consensus Guidelines for Periprocedural Management of Coagulation Status. J Vasc Interv Radiol. 2012;23(6):727–736.