Indications / Contraindications
Indications
- Relief of urinary obstruction (calculi, malignancy, stricture, retroperitoneal fibrosis)
- Infected obstructed collecting system (pyonephrosis) — URGENT
- Urinary diversion (ureteral injury, fistula, leak)
- Portal for endourologic procedures (nephrolithotomy, ureteral stent, rendezvous)
- Diagnostic (pressure studies, antegrade pyelography)
- Note: Hydronephrosis alone is NOT an indication — obstruction must be confirmed clinically + with imaging/labs
Contraindications
- Absolute: Uncorrectable coagulopathy (relative)
- Relative: INR <1.5 and platelets >50K generally acceptable
- Non-dilated system (increased technical difficulty, drops success to 82–96%)
- Horseshoe/ectopic/transplant kidney (modified approach required)
Pre-Procedure Checklist
Relevant Anatomy
Access Route
- Target: Posterior lower or middle pole calyx — standard approach
- Approach below the 12th rib to avoid pneumothorax. Stay above 12th rib = transpleural (avoid unless necessary)
- Access site: posterior axillary line, below 12th rib
- Brödel's line: Relatively avascular zone between anterior and posterior renal segments, 1 cm posterior to the lateral convex border — target zone for calyceal access
- Upper pole: Reserved for stone procedures requiring angled access; higher pneumothorax risk (below 11th rib)
- Transplant kidney: Typically RLQ iliac fossa, anterior approach with US guidance
Danger Structures
- Pleura: Upper pole access risk — below 11th rib = transpleural; approach below 12th rib
- Renal vasculature: Main renal artery enters hilum; lower pole posterior calyx approach avoids central vessels. Pseudoaneurysm/AV fistula = most feared vascular complication
- Colon: Retrorenal colon in ~10% of patients — check CT before access
- Liver/Spleen: Right-sided and left-sided lateral approaches respectively
- Subcostal nerve/vessels: Approach above rib edge (inferior margin)
- Infundibulopelvic veins: Large intrarenal veins can be crossed with small needles safely
Technique
Default RadCall approach · share your own below
Supplies
Steps
Position + imaging survey
Prep + sterile setup
Local anesthesia
Needle access
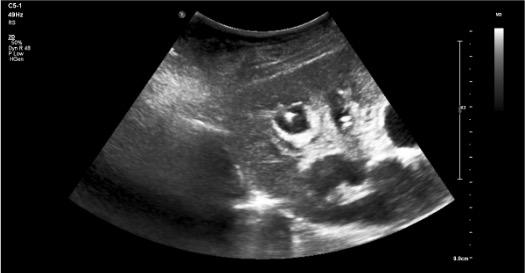
Wire placement
Tract dilation
Catheter placement
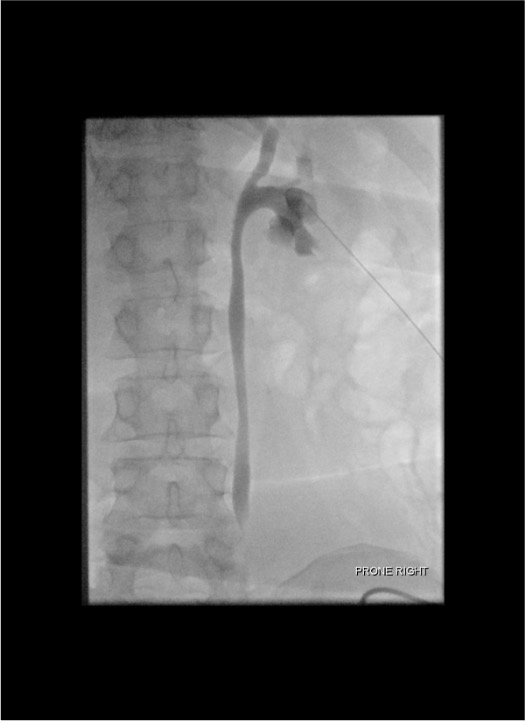
Secure + connect
Double-Stick Technique (Non-Dilated or Difficult Systems)
Use when the collecting system is minimally dilated and direct calyceal targeting is difficult. The first needle opacifies the system; the second needle accesses the target calyx under fluoroscopic guidance.
- 1First stick — opacification needle: Under US guidance, advance a 21G or 22G Chiba needle into the renal pelvis or any accessible calyx (precision not critical for this pass).
- 2Inject contrast: Slowly inject diluted iodinated contrast (1:1 with saline) through the first needle to opacify the collecting system under fluoroscopy. The pelvicalyceal anatomy is now visible.
- 3Identify target calyx: Under fluoroscopy, identify the posterior lower or middle pole calyx — look for the "end-on" calyx (appears as a circle, not a projection).
- 4Second stick — working needle: Under fluoroscopic guidance, advance an 18G or 21G access needle directly into the target calyx. The contrast outline makes targeting precise.
- 5Confirm access: Urine return or contrast aspiration from the working needle confirms calyceal entry. Proceed with standard wire and sheath placement.
- 6Remove first needle once the working wire is secured.
Troubleshooting
No urine return after needle insertion
Likely cause: Poorly dilated system, needle tip not in calyx, or decompressed collecting system.
Next step: In poorly dilated systems — try IV contrast 50–75 mL and wait 3–5 min for contrast excretion. Under fluoroscopic guidance with contrast in calyces, use triangulation for targeting. Consider cone-beam CT guidance for non-dilated systems.
Excessive bleeding after access
Likely cause: Arterial injury (bright red, pulsatile) vs. venous/collecting system blood (darker, non-pulsatile).
Next step: Distinguish vascular from renal pelvis blood. Bright red, pulsatile = arterial injury — do NOT dilate, apply pressure. Evaluate with urgent CT angiography → embolization if pseudoaneurysm confirmed.
Difficult wire navigation
Likely cause: Wire not traversing into ureter or encountering stone/stricture.
Next step: Use hydrophilic angled wire (Glidewire) + angled catheter (Cobra, vertebral) to navigate into ureter. For crossing obstructions, balloon dilation after traversal.
Transpleural access confirmed on fluoroscopy
Likely cause: Upper pole access with pleural transgression — air or contrast seen in pleural space.
Next step: If confirmed, obtain chest radiograph. If pneumothorax >10% or symptomatic, chest tube required. Modify future access to subcostal approach below 12th rib.
Dislodged catheter during dilation
Likely cause: Loss of wire control during dilator exchanges.
Next step: Re-access with fresh Chiba needle. Maintain super-stiff wire control throughout all dilation steps — do not let go of the wire. Consider placing a second wire as safety before dilating.
Complications
Immediate
- Hemorrhage (major ~1–4%) — most concerning; pseudoaneurysm/AV fistula → embolization
- Sepsis/bacteremia (1–10%) — most common cause of death; prophylactic antibiotics reduce risk
- Pneumothorax (1–4%) — if upper pole access; obtain CXR post-procedure
- Urine extravasation/urinoma — from inadvertent tract disruption
- Organ injury — liver, spleen, colon (retrorenal); rare but serious
Delayed
- Catheter occlusion/dislodgement — most common delayed issue; flush q8h with saline
- Pseudoaneurysm — delayed bleeding typically 2–4 weeks post-procedure; presents as gross hematuria
- Arteriovenous fistula — may close spontaneously; embolization if symptomatic
- Tract infection — skin/tract cellulitis; local wound care ± antibiotics
- Post-obstructive diuresis — after relief of chronic obstruction; monitor electrolytes
Post-Procedure Care
Monitoring
- Vitals q30 min × 2h post-procedure
- Monitor drainage output and color. Initial hematuria common (pinkish-red) — should clear in 24–48h. Frank blood = concerning
- Nephrostogram at 48–72h to confirm position and document drainage
- Drain flushing: 5–10 mL sterile saline q8h to maintain patency
- Urine culture from initial aspirate
Follow-up & Instructions
- Urology follow-up for definitive management planning
- Catheter exchange: every 3 months (Cope loop) to prevent encrustation
- Post-obstructive diuresis: Monitor electrolytes closely post-procedure. Diuresis >200 mL/h = replace 50–75% of output with IV saline
- Patient/family education: drain care, dressing changes, signs of dislodgement or infection
Critical Pearls
Catheter Management
Catheter Types & Exchange
- 8–10 Fr pigtail: Standard PCN; exchange every 3 months
- 14–18 Fr: For empyema/thick collections
- Large-bore: Complex stone access tracts
- Exchange earlier if: Occlusion, dislodgement, persistent infection, or encrustation
Output Norms
- Expected: 500–1500 mL/day after obstruction relief — track 24h output
- Urine leak around catheter: Check position + patency; flush. If dislodged, cover with sterile gauze and call IR immediately
- Catheter occlusion: Flush with 10 mL sterile saline gently. Do NOT force. If still occluded, exchange under fluoroscopy
- Minimal output: Rule out dislodgement, catheter kinking, or bladder outlet obstruction
Post-Obstructive Diuresis Protocol
| Urine Output Rate | Action | Additional Steps |
|---|---|---|
| <200 mL/h | Routine monitoring | BMP once at 6h |
| 200–500 mL/h | Replace 50–75% of output with IV normal saline | BMP q6h, strict I/O |
| >500 mL/h | Aggressive IVF replacement — 75% of hourly output | BMP q4–6h, consider ICU monitoring |
| Any rate with rising Cr or electrolyte abnormality | Nephrology consult | Adjust IVF composition based on lytes |
References & Resources
Key Guidelines
- CIRSE SoP: Nephrostomy & Ureteral Stenting → Ryan AG et al., CVIR 2026 · DOI
- SIR practice standard for PCN
- EAU guidelines on urological infections
Primary References
- Dyer RB, Regan JD, Kavanagh PV, Khatod EG, Chen MY, Zagoria RJ. Percutaneous nephrostomy with extensions of the technique: step by step. Radiographics. 2002;22(3):503–525.
- Ramchandani P, Cardella JF, Grassi CJ, et al; Society of Interventional Radiology Standards of Practice Committee. Quality improvement guidelines for percutaneous nephrostomy. J Vasc Interv Radiol. 2003;14(9 Pt 2):S277–S281.
- Dagli M, Ramchandani P. Percutaneous nephrostomy: technical aspects and indications. Semin Intervent Radiol. 2011;28(4):424–437.