Indications / Contraindications
Indications
- Lumbar radiculopathy (sciatica) — L4, L5, or S1 nerve root pain from disc herniation or foraminal stenosis; pain radiating below the knee in dermatomal pattern
- Neurogenic claudication from lumbar spinal stenosis (interlaminar approach preferred)
- Failed conservative management ≥ 6 weeks (NSAIDs, physical therapy, activity modification)
- Post-surgical radiculopathy (failed back surgery syndrome — epidural fibrosis, residual stenosis)
- Acute disc herniation with severe pain — bridge to natural resolution or surgery
- Transforaminal preferred: Single-level unilateral radiculopathy; level-specific steroid delivery; post-surgical anatomy; diagnostic injection to confirm target level
- Interlaminar preferred: Bilateral or multilevel symptoms; central stenosis; post-fusion anatomy; central disc herniations
Contraindications
- Absolute: Active spinal infection · Uncorrectable coagulopathy · Allergy to contrast or corticosteroids
- Anticoagulation (SIR Category 2 — moderate risk): INR ≤1.5, platelets ≥50K required. Warfarin: hold 5 days (verify INR ≤1.5 day-of). LMWH: hold 24h (therapeutic); hold 12h (prophylactic). DOACs: hold 24–48h. Heparin IV: hold 4–6h. Aspirin: continue. Clopidogrel / P2Y12 inhibitors: hold 5–7 days (epidural hematoma risk)
- Relative: Prior spinal fusion at target level (use CT guidance); uncontrolled diabetes; pregnancy; coagulopathy not fully correctable
- Note: Bridging anticoagulation is an individualized decision. Consult prescribing team for high-thrombotic-risk patients (mechanical heart valves, AF with CHA₂DS₂-VASc ≥4, VTE <3 months, recent coronary stent). NSAID / aspirin does NOT routinely need to be held for LESI per SIR guidelines
Pre-Procedure Checklist
Relevant Anatomy
Epidural Space
- Posterior epidural space at L3-5 is the target — widest at L3-4 (7–9 mm); posterior epidural fat provides "cushion" and drug distribution medium
- Bounded posteriorly by ligamentum flavum; anteriorly by posterior longitudinal ligament and posterior disc/vertebral body
- Spinal cord ends at L1-2 (conus medullaris) — below L2, only the cauda equina floats in the CSF; true intrathecal injection below L2 is less catastrophic than above, but still requires detection
- Anterior epidural space contains Batson's venous plexus — rich, valveless venous network; intravascular injection risk is real and must be checked before every medication injection
- Posterior epidural space can communicate between levels — but drug delivery is most targeted with transforaminal approach directly onto the affected nerve root
Transforaminal Safe Zone
- Safe triangle (subpedicular approach): Superior border = pedicle undersurface; inferior border (hypotenuse) = dorsal root ganglion; lateral border = lateral foraminal margin
- Needle target: 6 o'clock position of the pedicle on AP view — inferior and slightly medial; in the superior posterior neural foramen, posterior to the nerve root
- Kambin's triangle (alternative): inferior border = pedicle; superior border = dorsal root ganglion; medial border = articular process — useful when safe triangle is inaccessible (hardware)
- Artery of Adamkiewicz: Usually left T9-L1; can rarely extend to lumbar range — explains why particulate steroid into the radicular artery causes cord infarct
- Radicular arteries and venous plexuses are present within every neural foramen — aspirate and use live fluoroscopy with contrast before every injection
Technique
Default RadCall approach · share your own below
Supplies
Steps
Positioning + oblique view
Skin entry + needle advance
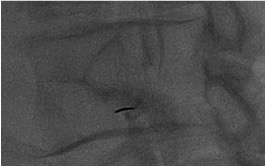
AP + lateral confirmation
Aspirate + contrast injection
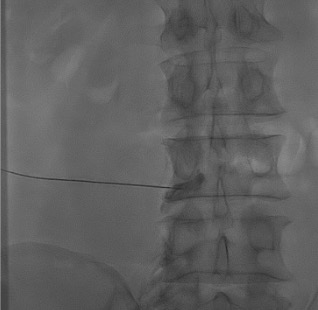
Inject steroid + anesthetic
Steps
Positioning + target level
Loss-of-resistance needle advance
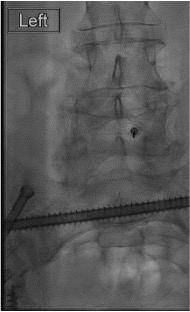
AP + lateral confirmation
Contrast injection — "Christmas tree"
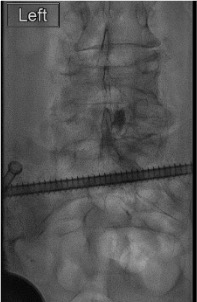
Inject steroid + anesthetic
Approach C — Caudal Epidural (Alternative)
Access via sacral hiatus with 22G spinal needle; confirm in sacral canal on lateral view; inject 10–15 mL dilute steroid/anesthetic. Useful for L5-S1 access in post-surgical patients or when superior approaches are inaccessible. Higher total drug volume required for cephalad spread to lumbar levels.
Troubleshooting
Intravascular contrast uptake — linear flow in vessel
Likely cause: Needle tip in epidural venous plexus (Batson's) or periforaminal radicular artery. More common with transforaminal approach and in post-surgical patients (distorted anatomy).
Next step: STOP injection immediately. Withdraw needle 1–2 mm; redirect slightly. Re-aspirate. Repeat contrast under live fluoroscopy before any steroid. If repeatable vascular uptake: try different trajectory. Consider switching to non-particulate dexamethasone if not already. Do NOT inject particulate steroid with any vascular uptake.
CSF return on aspiration (dural puncture)
Likely cause: Needle advanced too far anteriorly into the thecal sac. More common with interlaminar approach or when epidural fat is thin (prior surgery, spinal stenosis).
Next step: Do not inject steroid intrathecally. Withdraw needle back into epidural space and re-confirm with contrast. If intrathecal injection desired (rare — selective nerve root block): reduce volume to ≤1 mL and use preservative-free dexamethasone only. If accidental intrathecal: observe for spinal headache, total spinal anesthesia (bilateral leg weakness); most intrathecal dexamethasone injections at lumbar level are tolerated without permanent injury.
Unilateral contrast spread — drug not reaching target root
Likely cause: Midline septum or post-surgical adhesions limiting epidural spread in interlaminar approach; needle too far lateral in transforaminal.
Next step: For interlaminar: reposition needle to ipsilateral paramedian and repeat. Consider contralateral injection if bilateral symptoms. For transforaminal: confirm needle at 6 o'clock of pedicle; increasing volume slightly (up to 3 mL) can improve spread. Re-image with contrast before additional medication.
Severe radiculitis / paresthesias during injection
Likely cause: Needle tip too close to the nerve root (contact); or rapid injection into tightly stenosed foramen (pressure effect).
Next step: Stop injection immediately. Ask patient to describe: severe lancinating pain in dermatomal pattern = nerve contact → withdraw needle 1–2 mm. Diffuse burning = possible intravascular. Resume injection very slowly (0.5 mL/min maximum). If motor symptoms develop (quadriceps weakness): stop and monitor before considering additional medication.
Complications
Serious / Rare
- Spinal cord infarction — intravascular injection of particulate steroid into radicular artery; may cause paraplegia; prevention: live fluoroscopy + contrast before every steroid injection; use dexamethasone for all transforaminal approaches
- Epidural hematoma — rare (<1:150,000 epidurals); risk elevated with anticoagulation; presents with back pain + progressive leg weakness post-procedure; MRI urgently; neurosurgical consultation for decompression
- Epidural abscess — rare; fever, back pain, neurological deficits days–weeks post; MRI with contrast; IV antibiotics; surgical drainage if cord compression
- Total spinal anesthesia — inadvertent large-volume intrathecal injection; rapid bilateral sensory/motor block + hypotension; supportive care, airway management
Common / Minor
- Transient lower extremity weakness — from local anesthetic dorsal root block; resolves in 2–6h; patient must have a driver; observe until fully resolved before discharge
- Post-dural puncture headache — positional headache (worse upright, better supine) after accidental dural tap; conservative management (supine, caffeine, analgesics); blood patch if refractory
- Post-injection flare — temporary pain increase 1–3 days; resolves spontaneously; warn patient prior to discharge
- Hyperglycemia — steroid effect; especially in diabetics; monitor 24–48h; insulin adjustment if needed
- Vasovagal reaction — common; patient must remain supine during procedure; treat with fluids ± atropine
- Arachnoiditis — rare; associated with large volumes, intrathecal injection of particulate material, or preservatives; avoid by using preservative-free medications intrathecally
Post-Procedure Care
Recovery Monitoring
- Observe 30–60 min — assess for lower extremity weakness from local anesthetic; patient must fully recover motor function before discharge
- Motor block from bupivacaine: document and reassess q15–20 min; typically resolves within 60–90 min
- Cannot drive for 12–24 hours after procedure — arrange transportation in advance
- Monitor for signs of dural puncture: headache onset (positional, throbbing) — instruct patient to call if this develops
- Vitals q30 min × 1h in recovery; discharge when ambulating safely
Expected Response + Follow-up
- Steroid onset: 2–5 days after injection; full effect at 2 weeks
- Local anesthetic effect: Immediate but temporary (hours); may provide early symptom insight
- Reassess at 2–4 weeks. Document: degree of pain relief (%), functional improvement, return-to-activity milestones
- >50% relief with first injection — good predictor for continued benefit; may repeat if symptoms recur
- Series limit: Maximum 3 injections per 6-month period (evidence-based; beyond this, diminishing returns and increasing steroid-related side effects)
- If inadequate relief after 2 injections: reassess diagnosis; consider surgical consultation, alternative nerve root, or different pain source
Critical Pearls
References & Approach Comparison
Approach Comparison: Transforaminal vs. Interlaminar vs. Caudal
| Feature | Transforaminal | Interlaminar | Caudal |
|---|---|---|---|
| Best for | Single-level unilateral radiculopathy; level-specific delivery; post-surgical anatomy; diagnostic injection | Bilateral symptoms; central stenosis; multilevel disease; neurogenic claudication | L5-S1 when other approaches blocked; post-fusion; sacral radiculopathy |
| Steroid | Dexamethasone ONLY (non-particulate mandatory) | Triamcinolone or methylprednisolone (particulate acceptable) | Either acceptable; dilute with larger volume (10–15 mL) |
| Vascular risk | Higher — needle near foraminal vessels; live fluoro mandatory | Lower — posterior epidural space away from main vessels | Low — sacral canal far from cord; rich venous plexus still present |
| Volume | 2–3 mL total | 4–6 mL total | 10–15 mL total |
| Targeting precision | High — directly at nerve root axilla | Moderate — spreads bilaterally via posterior epidural space | Low — dilution over multiple levels; least precise |
| Guidance | Fluoroscopy (standard); CT for post-surgical or hardware | Fluoroscopy; CT for post-surgical | Fluoroscopy lateral view mandatory |
Citations
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. DOI: 10.1055/b000000387
- Filippiadis DK, Kelekis A. A review of current trends in spinal interventional procedures for the management of chronic spinal pain. Quant Imaging Med Surg. 2017;7(6):651–659.
- Mitchell JW. Radicular Pain Related to Disk Disease I: Transforaminal Injections. In: Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology. Thieme; 2024: Chap 26.
- Manchikanti L, et al. Epidural injections for lumbar radiculopathy or sciatica: a systematic review and meta-analysis. Pain Physician. 2020;23(4S):S185–S238.
- Bensler S, et al. Fluoroscopy-guided lumbar transforaminal epidural steroid injections: a systematic review and meta-analysis. Eur Radiol. 2018;28(2):618–629.
- SIR Standards of Practice Committee. Consensus Guidelines for Periprocedural Management of Coagulation Status and Hemostasis Risk. J Vasc Interv Radiol. 2012;23(6):727–736.
References & Resources
Key Guidelines
- ISIS Practice Guidelines
- ASIPP Evidence-Based Guidelines for LESI
- ACR Appropriateness Criteria
Primary References
- Manchikanti L et al. Comprehensive evidence-based guidelines for interventional techniques in the management of chronic spinal pain. Pain Physician. 2009;12(4):699-802.
- Abdi S et al. Epidural steroids in the management of chronic spinal pain: a systematic review. Pain Physician. 2007;10(1):185-212.
- Vad VB et al. Transforaminal epidural steroid injections in lumbosacral radiculopathy. Spine. 2002;27(1):11-16.