Indications & Patient Selection
Indications
- Chronic knee osteoarthritis (OA) pain — Kellgren-Lawrence (KL) grade II–IV, failed conservative therapy (NSAIDs, physical therapy, injections × 3 months)
- Positive diagnostic genicular nerve block (GNB) — ≥50% pain relief on diagnostic block is required and is the strongest predictor of successful RFA
- Post-total knee arthroplasty (TKA) persistent pain — genicular nerves may remain intact and continue to mediate pain after arthroplasty
- Failed intra-articular injections — patients with ongoing pain despite corticosteroid or hyaluronic acid injections
- Pain ≥ 6 months duration with functional impairment
Contraindications & Workup
- Absolute: Active knee joint infection · Uncorrectable coagulopathy · Planned TKA within 3 months · Pacemaker without cardiology clearance (bipolar RFA mode can be used with pacemaker after clearance)
- Relative: Prior ipsilateral knee surgery altering anatomy · Prior RFA at same site without adequate washout (≥6 months)
- Workup: Weight-bearing knee X-ray (KL grading) · Baseline VAS pain score · Functional assessment (WOMAC or KOOS) · Confirm pain ≥6 months · INR / anticoagulation status
- Note: OA grade does NOT predict RFA response — even KL IV patients can have excellent relief; response is predicted by GNB result, not imaging
Pre-Procedure Checklist
Relevant Anatomy
Three-Nerve Target Protocol
- Superior Medial Genicular Nerve (SMG): Runs along periosteum at the junction of the medial femoral condyle and medial femoral shaft — the "metaphyseal junction" on the medial side. Target: center of the notch between shaft and condyle on AP fluoroscopy.
- Superior Lateral Genicular Nerve (SLG): Junction of the lateral femoral condyle and lateral femoral shaft. Analogous position laterally. Note proximity to recurrent fibular (peroneal) nerve — do not target too far lateral or inferior.
- Inferior Medial Genicular Nerve (IMG): Junction of the medial tibial condyle and medial tibial shaft, just distal to the medial joint line. Most commonly under-targeted in failed RFA cases.
- Key rule: All three nerves run along periosteum at the epiphysis-diaphysis junction ("metaphyseal junction"). Periosteal contact = correct depth.
At-Risk Structures
- Saphenous nerve — runs medially near the SMG target; provides sensory innervation to the medial knee and distal leg. Injury (SMG too posterior) → medial knee and calf numbness.
- Recurrent fibular nerve (superficial peroneal branch) — near the SLG; injury → foot drop. Avoid ablating too far lateral or inferior at the SLG target.
- 5-nerve extension protocols add the Inferior Lateral Genicular nerve and Middle Genicular nerve — only recommended in experienced hands given increased peroneal nerve risk.
- Sensory stimulation (50 Hz, <0.5V) is the safety mechanism to confirm nerve location before ablation. Motor stimulation (2 Hz) rules out motor nerve proximity.
Technique
Default RadCall approach · share your own below
Supplies
Steps
Position and C-arm setup
Identify three targets under fluoroscopy
Advance 22G needle to periosteum
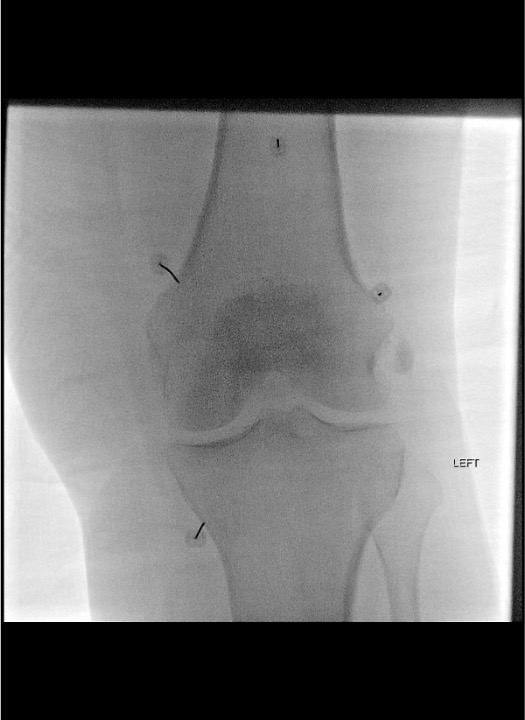
Inject lidocaine — small volume
Assess pain relief at 30 min
Steps
Position — same as diagnostic block
Place 18G RF cannula to periosteum
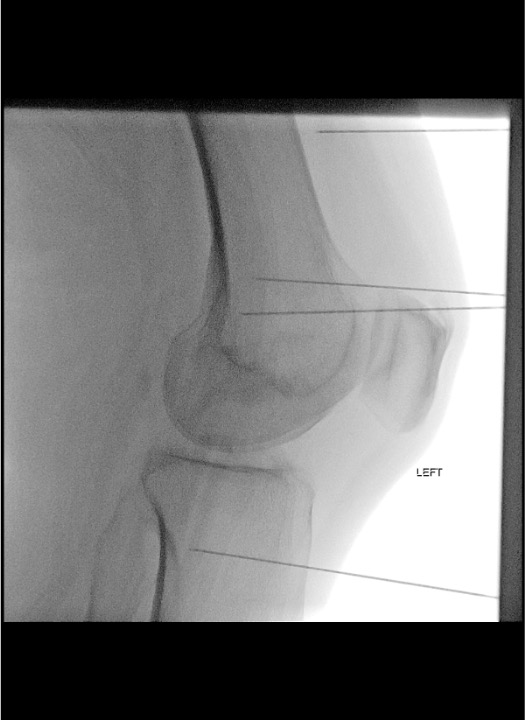
Sensory stimulation — 50 Hz
Motor stimulation — 2 Hz
Pre-ablation anesthesia
Radiofrequency ablation
Post-ablation injection at each site
Fluoroscopic Landmarks
Target Localization by View
| Target Nerve | AP View Landmark | Lateral View Confirmation | Key Pitfall |
|---|---|---|---|
| Superior Medial Genicular (SMG) | Medial femur — center of the "notch" between the femoral shaft and medial femoral condyle (metaphyseal junction) | Mid-depth of condyle; not anterior capsule, not posterior | Too posterior → saphenous nerve → medial numbness |
| Superior Lateral Genicular (SLG) | Lateral femur — analogous junction of lateral femoral shaft and lateral femoral condyle | Mid-depth of condyle laterally | Too lateral/inferior → peroneal nerve → foot drop risk |
| Inferior Medial Genicular (IMG) | Medial tibia — junction of medial tibial shaft and medial tibial condyle, just distal to the medial joint line | Anterior to fibular head level, mid-depth of tibial condyle | Most commonly missed target — ensure cannula is distal enough |
AP View Essentials
- All three metaphyseal junctions are visible on a single AP view of the knee
- SMG and IMG are on the medial side; SLG on the lateral side
- The RF cannula tip should overlay the periosteum at the junction — not on the joint space, not on the shaft alone
- Confirm position at each of the three sites before moving to lateral confirmation
Lateral View Essentials
- Superimpose condyles on lateral view for accurate depth assessment
- Tip should project at the mid-depth of the condyle
- Too anterior = anterior fat pad / anterior capsule — incorrect
- Too posterior = posterior capsule, popliteal vessels, neural structures — incorrect and dangerous
Troubleshooting
Paresthesia down leg or foot during sensory stimulation
Likely cause: RF cannula too posterior — near saphenous nerve (medial, leg paresthesia) or near recurrent fibular / peroneal nerve (lateral, foot or dorsum paresthesia).
Next step: Stop stimulation immediately. Withdraw cannula 2–3 mm and redirect anteriorly and slightly superiorly. Repeat sensory stimulation. Do NOT ablate until knee-specific paresthesia is reproduced at <0.5V. If paresthesia persists in the foot or lower leg, reposition significantly before retesting.
Motor response at low voltage during 2 Hz stimulation
Likely cause: RF cannula near a motor nerve — most often peroneal nerve at the SLG target (ankle dorsiflexion or eversion), or saphenous-adjacent motor branch at SMG.
Next step: Reposition cannula before ablation. Acceptable motor threshold = no motor response at <2× the sensory threshold. If motor firing occurs below this margin, redirect and retest both sensory and motor stimulation before proceeding.
Incomplete or short-lived pain relief after RFA
Likely cause: Most commonly the IMG was under-targeted (too proximal on the tibia, missing the metaphyseal junction). Less commonly, inadequate sensory stimulation confirmation before ablation.
Next step: Review fluoroscopic images — confirm IMG was at the medial tibial shaft-condyle junction distal to the joint line. Consider repeat RFA targeting 5 nerves (adding inferior lateral genicular and middle genicular). Repeat RFA is safe at ≥6 months.
Post-procedure pain flare (days 1–14)
Likely cause: Neuritis from thermal ablation of genicular nerve fibers — occurs in approximately 10–15% of patients; self-limited.
Next step: Reassure patient this is expected and transient. Manage with NSAIDs and ice. Resolves within 2 weeks in most patients. Post-ablation dexamethasone injection (at time of procedure) significantly reduces the incidence. Do not interpret early pain flare as procedure failure.
Complications
Immediate / Periprocedural
- Neuritis / post-procedure pain flare (10–15%) — most common complication; thermal reaction around ablated nerve; self-limited, resolves within 2 weeks; mitigated by post-ablation dexamethasone + bupivacaine injection
- Saphenous nerve injury — SMG cannula placed too posterior → medial knee and calf numbness / dysesthesia; usually temporary; avoid by confirming no leg paresthesia at sensory stimulation and maintaining anterior trajectory
- Peroneal nerve injury / foot drop — SLG cannula placed too lateral or inferior → ankle dorsiflexion weakness; most serious complication; avoid by strict motor stimulation threshold testing and conservative SLG targeting
- Skin burn — rare with proper technique; RF tip must not contact dermis; ensure adequate needle depth before ablation
Delayed
- Infection — rare (<1%); sterile technique essential; present as worsening pain, warmth, fever; treat with antibiotics; joint aspiration and culture if septic arthritis suspected
- Incomplete ablation — inadequate lesion size (too low temperature or too short duration); protocol-compliant technique (80°C × 90 sec or cooled tip 55°C × 150 sec) minimizes this; repeat RFA safe at ≥6 months
- Limited duration of effect — nerves regenerate over 6–12 months; pain recurrence expected; repeat RFA is safe and effective and can be offered when pain returns
- Hematoma — rare; SIR Category 1 procedure; usually self-limited; compressive dressing and observation
Critical Pearls
References & Community Cards
Outcome Data Summary
| Timepoint | KOOS Score | WOMAC Score | VAS Pain |
|---|---|---|---|
| Baseline | 16.7 | 23 | 9–10 |
| 2 weeks | 81 | 65 | 4 |
| 1 month | 84 | 65 | 2 |
| 3 months | 86 | 65 | 1 |
| 6 months | 91 | 82 | 0 |
Data from Gonzalez FM, Broida SE, Kokabi N (Prologo & Ray, Thieme 2024) — cooled RFA, SIFK patient. KOOS = Knee Injury and Osteoarthritis Outcome Score; WOMAC = Western Ontario and McMaster Universities Osteoarthritis Index; VAS = Visual Analog Scale.
Citations
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology: A Case-Based Approach. Thieme; 2024. Ch. 34: Gonzalez FM, Broida SE, Kokabi N — Nerve Ablations I (Genicular RF).
- Choi WJ, Hwang SJ, Song JG, et al. Radiofrequency treatment relieves chronic knee osteoarthritis pain: a double-blind randomized controlled trial. Pain. 2011;152(3):481–487.
- Jamison DE, Cohen SP. Radiofrequency techniques to treat chronic knee pain: a comprehensive review of anatomy, effectiveness, treatment parameters, and patient selection. J Pain Res. 2018;11:1879–1888.
- Sayyid S, Younan Y, Sharma G, et al. Subchondral insufficiency fracture of the knee: grading, risk factors, and outcome. Skeletal Radiology. 2019;48(12):1961–1974.
- SIR Standards of Practice Committee. Consensus Guidelines for Periprocedural Management of Coagulation Status. J Vasc Interv Radiol. 2012;23(6):727–736.
References & Resources
Key Guidelines
- ISIS Practice Guidelines
- ASIPP Systematic Review on Genicular Nerve RFA
- ACR Appropriateness Criteria
Primary References
- Choi WJ et al. Radiofrequency treatment relieves chronic knee osteoarthritis pain: a double-blind randomized controlled trial. Pain. 2011;152(3):481-487.
- Prologo JD, Ray CE Jr., eds. Advanced Pain Management in Interventional Radiology. Thieme; 2024. Ch. 34: Genicular Nerve Radiofrequency Ablation.
- Iannaccone F et al. A meta-analysis of clinical effectiveness of radiofrequency neurotomy for facet and sacroiliac joint pain. Pain Physician. 2012;15(4):297-304.